

Why Is My Dog Or Cat Breathing Abnormally Or Panting?
Ron Hines DVM PhD
 See What Normal Blood & Urine Values Are
See What Normal Blood & Urine Values Are
 Causes Of Most Abnormal Blood & Urine Tests
Causes Of Most Abnormal Blood & Urine Tests
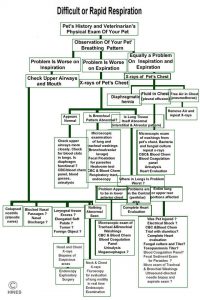 Click to see how your vet might proceed
Click to see how your vet might proceed
Veterinary terms are confusing, but cats and dogs that breath too fast are said to have tachypnea or hyperpnea (or to be hyperventilating). Those breaths are usually also shallower than they normally would be. Pets that take deeper breaths than normal are said to have hyperpnea. Pets that have labored, difficult respiration are said to have dyspnea. Those that breath too slow are said to have Bradypnea (a term that is almost never used). More than one term often applies to the situation your pet is experiencing.
How and how fast your dog or cat breathes is controlled by a group of very complex regulatory factors. It is such a complicated process that, to this day, how it works is not fully agreed upon or understood. However, physiologist do know that two control centers exist in your pet’s brain stem (it’s medulla). One is for inspiration and one is for expiration. More poorly understood regulation occurs in your pet’s spinal cord and two sensors, the carotid and aortic bodies, monitor oxygen and carbon dioxide levels in your pet’s blood stream. They, too, relay that information to your pet’s medulla. When all is well, all of them work together like an orchestra to keep your dog or cat’s body well oxygenated and to expel waste carbon dioxide through its lungs. When it fails, pets with too much carbon dioxide and too little oxygen in their bodies are said to be hypercapnic and hypoxic.
Labored breathing, dyspnea, is always an emergency. It is one of the scariest situations that pet owners and veterinarians face. These pets are right on the edge in their ability to meeting their oxygen need. The least bit of excitement can throw them over that edge causing them to collapse. They need supplemental oxygen, and they need it fast – either by face mask or oxygen chamber. They will do better when cool on the way to your nearest animal hospital. If your pet has cardiac, lung or seizure issues, it is safest to keep an emergency source of oxygen at home.
Being an emergency situation, many dyspneic pets need immediate veterinary attention. So most vets dispense with protocol before asking you when did this begin? Has it happened in the past? Has your pet been coughing or sneezing or exhibited other abnormal behaviors? Is there a history of recent trauma or electrical cord chewing? What about toxic product exposures, allergies, stings, current medications your pet receives, etc.? Often your dog or cat’s physical exam needs to be done in stages so as not to over stress the animal. Vets and their nurses keep tracheal tubes at the ready and cut down kits to find collapsed veins, should things take a turn for the worse.
Panting
Dogs and cats that pant can be attempting to lower their body temperature or just excited. In dogs that is common. In cats, it rarely is. Normal reasons for panting include exertion, stress, heat and as I mentioned, excitement. Overweight, long haired and short-nosed pets are more susceptible to heat-related causes. High humidity compounds the tendency to pant. Physical reasons for panting in dogs and cats include fever, heatstroke and pain as well as blood, heart and lung-related issues. Medication overdoses and toxic exposures to things like chocolate or insecticide need to be ruled out as well.
How Veterinarian Go About Determining The Cause
Observing your pet in the exam room is sufficient for your veterinarian to recognize cases of dyspnea. Receptionists need to be instructed in that too. If an emergency, your vet is likely to first check your pet gums and tongue to see if it is cyanotic. Its CRT time might be slow. It might need some immediate some oxygen. Improvement with supplemental oxygen also helps rule out anxiety or pain as the underlying cause. Your veterinarian will most likely then reach for his/her stethoscope. What vets hears through that marvelous contraption tells us a lot: heart situations, fluid in the lungs or chest, abnormal lung sounds, decreased audibility and more. Looking down your pet’s throat for obstructions and lodged items and examining its mouth and wind pipe are quite important. All must be done gingerly in pets that are on the brink of collapse. Extra staff, endotracheal tubes and “cut-down” kits are best brought close at hand when pets are having trouble breathing.
As your veterinarian proceeds, some things he/she might be looking for are narrow nostrils and nasal passages common in brachiocephalic breeds (=stenotic nares), crusts and discharges that are evidence of infections of the respiratory system, collapsing windpipes in toy breeds, laryngeal paralysis in larger breeds. Fever needs to be ruled out as the cause. X-rays are probably the next step. Radiographs allow your vet to visualize your pet’s heart and lungs – the two most common sites of serious respiratory problems. Issues such as an enlarged heart, organs displaced from their proper positions, fluid in the lungs or surrounding them, chest tumors, fractured ribs, diaphragmatic hernias or air in the chest might be readily visible on those x-rays or suggestive of the cause of your dog or cat’s breathing problem. Even when the cause is determined, lab work is often required.
Shock also causes rapid shallow respiration. Your pet’s CRT time, body temperature and pulse strength all help confirm or rule out a shock-related breathing problem. When confirmed or suspected, those pets are usually given intravenous fluids customized to meet their needs.
Specific Reasons For Panting Or Labored Breathing
You can read a flow chart that veterinarians use to sort out possible causes of panting here:
Heart Failure
In young adult and middle-aged dogs in South Texas where I practice, the most common cause of respiratory distress combined with declining health is advanced heartworm disease. But when heart failure occurs in dogs in areas where the disease is not as common or in dogs that are taking monthly heartworm preventatives, the most common cause is mitral heart valve disease.
Veterinary cardiologists often ask their clients to monitor the number of breath’s per minute that their pet takes while it is relaxing at home or sleeping. Your pet’s respiratory or breathing rate while it is sleeping is usually a bit slower than its resting respiratory rate. Dogs with rates between 25 and 30 breaths per minute rarely have congestive heart problems (clinical heart disease) as the underlying cause of their increased breathing rate. That does not mean that they are free of heart problems. It just means that heart problems if present have not reached the point where they would affect respiration. Resting breathing rates in cats are quite variable; but normal cats take less than 30-40 breaths per minute.
You can read a study of respiratory rate as a sign of heart disease here:  (ask for Ohad2013.pdf)
(ask for Ohad2013.pdf)
Another heart problem, hypertrophic cardiomyopathy (HCM), can also be the cause of rapid breathing.
Chest Trauma, Auto Accidents, Dog And Cat Fights
Depending on the damage done, these dogs and cats often exhibit shallow rapid breathing, shock or the labored breathing common to torn diaphragms, rib fractures, lung bruising (contusions) free blood surrounding the lungs (=hemothorax) or air in their chest (=pneumothorax). Sometimes their blood loss was so great that the underlying cause of their rapid breathing is blood loss anemia. Occasionally, the shock and circulatory collapse that follows these severe traumas begins a coagulation cascade leading to intravascular coagulation (DIC). Occasionally, when the blow was to the head, respiration will actually be slower than normal due to brain trauma that affected the pet’s brain respiratory control centers.
Poor Oxygen Perfusion Of Your Pet’s Body
Trauma is by no means the only cause of shock that causes rapid breathing. Sudden allergy events (=anaphylaxis), overwhelming infections (=septicemia) and electrical shocks all produce similar effects. In all forms of shock, blood pressure and the flow of blood throughout your pet’s body drops to critically low levels (=circulatory collapse). In these situations, your pet becomes hypovolemic (=not enough volume of blood plasma fluid in its circulatory system). Its body becomes starved for oxygen and its blood carbon dioxide level increases. Cells cannot live without oxygen. Too much carbon dioxide in circulation leads to life-threatening changes in your pet’s body pH (= metabolic acidosis). When that occurs your pet needs immediate attention. Other signs of shock include pale gums, slowed CRT, cool extremities (legs, ears, tail) and a weak pulse.
Blood Acid-Base Disorders
The health of all living creatures depends on their bodies operating within a very narrow range of acidity. Generally, that is just above the neutral point of pH 7. Below pH 7 is an acidic pH, above pH 7 is a basic pH. So, your pet’s blood should be slightly basic. Healthy cats and dogs have a blood pH of 7.35 to 7.45. All forms of shock tend to make your pet’s blood more acidic – that is, to cause its blood pH to go down. That situation is also called metabolic acidosis. Your pet relies heavily on its kidneys to maintain a proper blood acidity, so dogs and cats in late kidney failure often share these issues. The ketoacidosis that accompanies uncontrolled diabetes in dogs and cats can also cause rapid respiration. Hypoglycemia that occurs when too large an insulin dose is given has the same effect.
Anemia
Anemia makes it harder for your pet to obtain sufficient oxygen. Consequently, it will breathe faster. The two most common causes of anemia in the tropical humid region of the USA where I live are heavy infestation with intestinal hookworms and heavy flea infestations. Hookworm anemia is more likely to occur in young, growing dogs and cats that have not yet developed age-related resistance to the parasite. Serious flea infestations occur in puppies and kittens because they are often confined to small areas that favor flea reproduction.
A second type of anemia occurs more frequently in mature dogs and occasionally cats. In that form of anemia, your pet’s immune system mistakenly produces antibodies that destroy its own red blood cells. This phenomenon is called immune-mediated anemia or autoimmune hemolytic anemia. Red blood cells are being destroyed in these pets while they are still in circulation in the blood stream. Much of this unfortunate action occurs in the dog or cat’s spleen. Pets with this form of anemia are often weak and pale. Their blood bilirubin values are high. Some also develop bleeding disorders that add to their anemia due to lowered thrombocyte counts. Rapid breathing and elevated heart rate are very common in cases of autoimmune hemolytic anemia.
Feline Infectious Peritonitis
Feline Infectious Peritonitis is caused by a mutant form of the cat coronavirus. Symptoms of the disease vary depend on what area of your cat’s body is most affected. When it is the coverings of the cat’s lungs and chest wall (its pleura), excess fluid and inflammation prevent proper lung expansion. It is common for those unfortunate cats to breathe rapidly or even pant. When FIP fluid builds up in a cat’s abdomen, it also eventually interferes respiration because increased abdominal fluid pressure hinders the movement of the diaphragm.
Blood Parasites
The two most common ones are the Mycoplasma haemofelis (aka haemobartonella) parasite of cats and Babesia canis of dogs. The first, M. haemofelis is primarily transmitted by fleas, the second B. canis is transmitted by the brown dog tick. Both can cause your pet to become anemic. If that anemia is severe, your pet’s respiratory rate will be increased.
Upper Airway Obstructions And/Or A Collapsing Trachea
Some dogs have been intentionally bred for human fancy to have narrow, distorted airways (nose, nasal passages, pharynx and larynx). Those are the breeds that tend to snore. They are called the brachiocephalic breeds. Flat faced cats are not exempt. When these pets have any sort of inflammation or swelling in their upper respiratory tract (such as in kennel cough, allergies, smoke exposure, etc.) they have difficulty obtaining sufficient oxygen. Because their airflow and ability to obtain oxygen is marginal even in the best of situations, they are also the breeds to suffer first from heat stroke, heat or exercise exhaustion. In all of those situations they tend to breathe faster and more laboriously. Similar situations can occur in non-brachycephalic breeds when tumors, polyps, or laryngeal paralysis occur.
A second upper airways issue is most common in toy breeds (Yorkshire terriers, poodles, Pomeranians etc.). It is the presence of a trachea that does not maintain its normal oval shape. That occurs when the cartilage rings that support its shape are too flabby. Most pets with this problem were born with that tendency. But in a few, perhaps the cartilage was weakened by Cushing’s disease. If that theory is true, over use of corticosteroid medications might produce the same problem. Both the disease and the medications also produce fluid retention and encourage obesity. So, how and if they play a part in breathing issues is yet to be determined. In any case, when tracheal problems becomes so serious as to limit your pet’s ability to take in sufficient air, labored breathing, and occasionally more rapid breathing might occur. A hacking cough after exercise or pressing on the trachea would precede that. This problem can become so serious as to cause the pet to faint or turn blue (cyanosis). You can read more about how veterinarians approach this problem here & here.
Feline Asthma, Feline Bronchial And Lower Airway Disease
The signs of asthma in cats can be quite similar to the signs of heartworm disease in cats. It can also be confused with the signs associated with the occasional outdoor cat infected with lungworms.
Some cats, particularly purebreds, develop lung-directed allergies that inflame and narrow the small passageways within their lungs (their bronchial tree). This results in the narrowing of the airways and causes breathing difficulty (dyspnea), especially when exhaling. These cats often breath with their mouth open. It is common for their chest and tummy to heave – almost as if they were attempting to pass a hairball. During paroxysms (sudden recurrences) of rapid, shallow breathing, you might hear whistling sounds as your cat exhales. These bouts occur from only occasionally too frequently. Their severity varies from mild to a life-threatening medical emergency. Smoke inhalation or bronchopneumonia can cause similar symptoms.
pyothorax
Some dogs and cats develop chest infections that produce exudates that occupy the space surrounding their lungs (their pleural space) rather than within their lungs themselves. Veterinarians call that pyothorax. This problem almost never occurs without an underlying cause. Usually, there is an underlying health issue that has decreased your pet’s ability to fight infections. In cats, it might be an underlying feline leukemia or feline immunodeficiency virus. In dogs, it might be severe malnutrition, stress, or canine distemper. In puppies and kittens, it might be a failure of their mother to pass on sufficient immunity (antibodies) in her milk colostrum. Occasionally, a penetrating thorn, sharp dry grass seed or other sharp object allows an infection to enter the chest. In other cases infection appears to get to the plural space from the blood stream. These pets all have breathing problems, both in rate (increased) and in effort (dyspnea).
Pulmonary Edema/ Due To Anaphylaxis, Vaccines Or Other Drug Reactions
All of these situations liberate inflammatory cytokines, natural body chemicals that cause the small blood vessels throughout your pet’s body to leak fluid (increased vascular permeability). Your pet’s lungs, being very vascular, have the potential to fill with that fluid (pulmonary edema). When that same fluid leaks under your pet’s skin, it causes a bumpy puffiness called angioedema.
Circulatory Failure
Respiratory rate also increases when your pet’s heart is failing. In those cases, the flow of blood through your pet’s lungs is too slow and some leaks into the tiny chambers reserved for oxygen transfer and carbon dioxide elimination (=pulmonary edema). Pulmonary edema commonly occurs in cats with cardiomyopathy and dogs with cardiomyopathy. Some other possible causes are sudden (acute) pancreatic shock, snake bite, insecticide poisoning, stomach/splenic torsions, parvovirus, infection, a very low blood albumen level – usually due to your pet’s kidneys leaking albumin into its urine, overzealous IV fluid administration or uremia. For poorly understood reasons, electrical shocks, such as your pet gnawing on an extension cord, can start this process as well (neurogenic edema). Your pet’s heartbeat will be rapid and its pulse weak. Sometimes, foamy liquid from the lungs is coughed up as well. These are medical emergencies. Whenever there is excess fluid or fluid in the wrong places, diuretics such as Lasix® are commonly dispensed.
Diaphragmatic Hernias
When a cat or dog receives a severe blow to its central body such as in a traffic accident, the sudden increased pressure on its abdomen and thorax can tear its diaphragm. Generally, the diaphragm rips where it is attached to the chest wall. Without an intact diaphragm, dogs and cats have great difficulty breathing. In an effort to compensate, they shift their normal breathing muscle movement from their chest (intercostal muscles) to their abdomen muscles (rectus abdominis, etc.). Their breathing becomes labored and rapid. On rare occasion, a pet is born with an incomplete diaphragm that allows the space surrounding its heart (the pericardial sac) to communicate with its abdominal contents (a pericardial/peritoneal hernia). In that condition, bloat or other abdominal pressure can force its abdominal organs forward through that tunnel and into the pet’s chest. That severely limits the pet’s ability to breathe normally.
Cardiomyopathy – Heart Failure Hypoxia
I mentioned this problem earlier. Veterinarians do not know why some cats and dogs develop sudden heart muscle damage or cardiomyopathy. In cats there was a time that it was associated with a low taurine amino acid intake. That deficiency may have been associated with similar heart problems in dogs as well. Since that discovery, pet food manufactures add taurine to their finished products. Read more about this problem in dogs here and in cats here. Should you have a ferret, go here.
Hyperthyroidism
Hyperthyroidism in older cats is quite common. Hyperthyroidism is quite rare in dogs. I have never seen a case. It has, however, been reported that in dogs that were fed large amounts of raw beef necks which included the cow’s thyroid gland, hyperthyroidism occurred. When hyperthyroidism occurs, metabolism speeds up. Although weight loss and hyperactivity are the most likely signs that a pet owner would notice, hyperthyroid pets might also have an increased pulse rate, increased respiratory rate or panting.
Pulmonary Hypertension
This is a particular localized form of high blood pressure that affects mainly the blood vessels that run to and from your pet’s lungs and within its lungs themselves (the total pulmonary vasculature). Any of a number of problems that impede (obstruct) the flow of blood through your pet’s lungs can cause this condition. One of its signs is shortness of breath during and after exertion. Read more about that problem here.
Aspiration Pneumonia
This particular form of pneumonia occurs when food or liquid accidentally enters your dog or cat’s lungs rather than passing down its esophagus into its stomach. I see it most frequently in kittens and puppies that are still being bottle-fed. But it can also occur due to vomiting during anesthesia, coma or due to near drowning. Because your pet’s body has no effective ways to expel foreign material once it is deep within the lungs, cases can be very difficult to fully cure. Bacteria soon take advantage of the situation. The foreign material also gives those bacteria refuge from the pet’s immune system macrophages that would normally destroy them. Although coughing is the most common symptom, about half the dogs with aspiration pneumonia also experience rapid breathing (tachypnea) and fever. Dyspnea (labored breathing) is more common in infant pets. Those little creatures cannot elevate their body temperature effectively – so they rarely if ever run a fever in this situation.
Lung Tumors Or mediastinal (=Central Chest) Disease
Your pet’s mediastinum is the curtain of tissue that divides the two sides of its chest (right from left). It normally contains your pet’s thymus gland, heart, aorta, trachea, esophagus, vagus nerve, and some of its lymph nodes. Your pet’s mediastinum is different from the Wikipedia description in an important way; in us humans, this curtain of tissues is complete and isolates each side of the chest. In dogs and cats it is incomplete – so problems occurring on one side often spread to the other. Anything that makes the mediastinal area swell, decreases the area for your pet’s lungs to expand and makes its respiration difficult. Anything that occupies space within or between the lobes of the lungs has the same effect. Tumors are the most common space-occupying masses in both locations. Besides respiratory distress, associated problems in this area cause exercise intolerance, excessive panting and coughing.
While pets with an upper airways obstruction of their mouth, throat or trachea tend to have difficulty inhaling, pets with lung or mediastinal disease often have problems during inhalation and exhalation. Those with problems that include fluid or edema in the chest and lungs tend to have most difficulty during exhalation (see the chart at the top of this page). Cats hide these signs better than dogs do and tend to be brought to veterinarians later – when the situation is likely to be more critical. Some cats arrive in a frightened and agitated state and may simply keel over and pass away while the vet and his/her nurses struggle to examine them. So, oxygen needs to be at the ready.
Patent ductus arteriosus (PDA) Foramen Ovale
When your puppy or kitten was in its mother’s womb, there was no need for large volumes of blood passing through its lungs because their lungs were not exposed to the oxygen in air. At that stage of life, your kitten or puppy relied on its umbilical cord and its mother’s placenta, lungs and urination to meet its oxygen needs and to discharge carbon dioxide and other wastes. To bypass its lungs, your embryonic pet had a channel (a shunt) between the vessels that led to its lungs and the main blood vessel supplying its body (the aorta). This channel allowed the infant’s blood to bypass its lungs. That channel is called the ductus arteriosus. The fetal pet had another hole between the left and the right side of its heart that also helped bypass its lungs, the foramen ovale. At birth, both those channels are supposed to close naturally. They usually do close during the first day after birth. Occasionally, one or the other or both don’t close. When that happens, your pet’s lungs cannot provide enough oxygen. If you are fortunate, your veterinarian will picked up the distinctive heart murmur that this defect causes on the pet’s first exam. But many cases are missed. In those cases, dogs and cats are usually presented breathing rapidly These problems can often be corrected surgically at specialized veterinary facilities. For unknown reasons, female dogs have twice the number of this problem than males. Dog breeds more prone to this condition include poodles, bichons, Maltese, Pomeranians, Chihuahuas, collies, spaniels, keeshond, and Shetland sheepdogs. But any breed can suffer from the problem. The problem produces a distinctive heart murmur. When I was learning to be a veterinarian, they called this a “machine murmur”. You can hear the sound your vet might hear through a stethoscope here.
Ingestion of Stimulants
Some dogs and a few cats love to munch on forbidden items. I suppose they think we save the good food for ourselves. Should your pet manage to eat a stimulant such as Adderall® used to treat ADHD (read here), or eat substantial amounts of chocolate (read here) or partake of marijuana-containing products (read here) their respiratory rate will be very rapid. Many insecticides, although not thought of as stimulants, when applied in excess, licked or swallowed can have a similar effect. All can be medical emergencies because they can rapidly progress to seizures and death. Late in these poisoning cases, a pet’s respiratory rate can actually be depressed.
Transfusion Reactions
The rare transfusion of a mismatched blood unit (or one that for reasons not understood should have been compatible but wasn’t) to a dog or a cat can cause rapid respiration and a rapid heart rate. Most of these reactions are mild or moderate and transient. Most can be successfully managed by your veterinarian.
The Rare And Extremely Rare Causes:
Primary Ciliary Dyskinesia Syndrome aka Immotile Cilia Syndrome
This is a genetic problem that occasionally occurs in dogs, people and mice. However, something similar occasionally occurs in pets that suffer from long-term respiratory tract infections. We all rely on the wave-like action of tiny cilia (hair-like projections on the surface of cells that line your pet’s respiratory system) to move dust, dirt, pathogens and secretions out of our lungs. In rare instances in dogs, these cilia fail to function properly. That leads to bronchitis, pneumonia and sinusitis. When the lungs and airways of these pets can no longer function adequately, the pet’s respiration will be negatively affected. They will breathe faster, and their breathing will be more labored. Primary Ciliary Dyskinesia (PCD) has been reported in doberman pinchers, Newfoundlands, bichon frisé, Old English sheepdogs, English springer spaniels, golden retrievers, English pointers, Gordon and English setters, and rottweilers.
Histoplasmosis And Blastomycosis
Histoplasma and Blastomyces are two fungi that occasionally become established in the lungs of dogs – and much less frequently in cats. These fungi are quite content to live free in the soil. They both prefer moist conditions, moderated temperatures and rich, acidic soils or compost. They are often found in soils contaminated with bat or bird droppings. Stale, motionless air aids in their transfer. All of us and our pets have probably all been exposed to these fungal spores because they are so common in our environment. In humans, over 95% of the time our immune systems rapidly destroy these organisms once they have been inhaled. That is probably true in our pets as well. But in pets and people that are chronically stressed or have weakened immune systems, those fungi can prosper in the lungs. It is also thought that living or visiting highly contaminated areas sometimes exposes pets and people to enough fungal spores to override our natural defenses. When that occurs, these fungi germinate in the lungs and have the potential to form granulomas. Once that situation has occurred it is difficult to obtain permanent cures. Those pets develop weight loss, weakness, low-grade fevers and shortness of breath.
Why Your Dog Or Cat Might Have A Slow Respiratory Rate
All the conditions I listed for an abnormally low body temperature can be reasons pets breathe abnormally slow (=Bradypnea a word nobody uses). It could also be because your pet was exposed to very cold temperatures. It could be major traumatic blood loss. It could be brain trauma and swelling resulting from a car accident or a fall. Your pet could have reached the end-stage of many different major organ failures. The end stage of so many diseases is circulatory collapse and a downward trend in respiratory rate and body temperature. With emergency treatment, some of these can be reversed. But many of them are a downward spiral for which your veterinarian has no cure.
Less commonly, hypothyroidism will cause a slower than normal respiratory rate in dogs. Hypothyroidism is an extremely rare event in cats. All forms of depressants, tranquilizers, opioid narcotics and anesthetic medications will slow your pet’s respiratory rate when given in overly large doses. So can drugs given for heart rhythm disorders or high blood pressure. Sometimes the dose your veterinarian prescribed was the proper dose and an unwanted event still occurred. That is because some dogs and cats are deficient in certain enzymes such as P450 that keep blood levels of these products stable. In other pets the unexpected decrease in breathing rate was due to unrecognized liver disease. (read here) That is why pre-surgical blood analysis is always the best option.
Dogs, cats and humans in the midst of an epileptic seizure can have difficulty breathing or stop breathing altogether (=apnea) (read here). Brain centers controlling respiration can be affected during seizures or the diaphragm muscles can become so rigid and non-functional that breathing cannot occur normally. The most dangerous situation is when seizure follows seizure or in grand mal rigidity. Dogs can also experience a wide variety of sleep disorders that affect their nighttime and nap respiration (read here)
Organophosphate insecticide exposure can increase respiratory rate. But exposure to these products can also cause diaphragmatic paralysis that prevents normal breathing, (read here) through its effect on the phrenic nerve that controls the diaphragm. These compounds can even be responsible for long-term damage to normal respiration. (read here)
Complementary Tests That Come To Mind
You can see from the length of this article that the causes of abnormal respiration are too many for me to name or for me to name tests for. You brought your cat or your dog to your veterinarian because you were worried that it was breathing abnormally. Your vet was trained to see the other less obvious abnormalities that will guide him or her in the proper choice of tests.
DxMe
You are on the Vetspace animal health website
Visiting the products that you see displayed on this website help pay the cost of keeping these articles on the Internet.








