The SDMA Test – What Abnormal Results Mean And What They Don’t Mean
Ron Hines DVM PhD
 Kidney Disease In Your Dog & Cat- Its Diagnosis And Treatment
Kidney Disease In Your Dog & Cat- Its Diagnosis And Treatment
 Kidney Problems In Your Cat – Renal Failure (CRF)
Kidney Problems In Your Cat – Renal Failure (CRF)
 Cat & Dog Owner Comments On The SDMA Test
Cat & Dog Owner Comments On The SDMA Test
Through 2023, human nephrologists at the National Institutes of Health, the Mayo Clinic and the National Kidney Foundation do not believe that the SDMA test is of much value in evaluating the seriousness of kidney disease. They feel that at this time, blood creatinine level and measuring protein leakage into urine, although imperfect tests, are still the most reliable ways that your kidney health can be judged. There is no evidence that dogs and cats are any different.
I am going to tell you everything that I know about your pet’s SDMA test results. For many of you, it’s considerably more than you want to know. Most of my articles are like that. But if you’re an in-depth medical research junkie, or want unbiased in-depth knowledge of your pet’s health issue, you can read the whole thing. You can also ask me for the full texts of all the articles I cite in any of my articles. Otherwise, just go to your pet’s treatment options.
The SDMA test for dogs and cats became available in the United States and Canada in 2015. Idexx Laboratories developed and patented the test. In Europe, the test was rolled out in 2016. Idexx offers their SDMA test as a new and more accurate way to judge your dog and cat’s kidney health. Their main selling point is their claim that the test discovers kidney problems earlier than the tests your veterinarian relied upon in the past. No independent research has ever confirmed that. In this article, I hope to give you a more balanced, independent picture of what scientists know about SDMA, what they do not know, and factors other than kidney disease that might make your cat and dog’s SDMA level go up or down. The only independent 2020 article that examined the SDMA test’s value was in your cat’s cousin, the cheetah. Cheetahs are even more likely to develop the same kidney issues (CKD) that your cat does. (read here) In that 2020 independent study, BUN and creatinine levels were considerably more accurate in measuring kidney health than was SDMA. (read here) There was an earlier cheetah kidney study in 2018. Although it measured SDMA and creatinine levels in cheetahs with kidney and other health issues, it did not compare them to cheetahs without kidney issues. That study’s only conclusion was that SDMA and creatinine tended to go up at about the same time. As for independence, five of the ten authors were employees of Idexx. (read here). If you want more than their abstracts, just ask me for them.
Veterinarians have traditionally relied on your pet’s blood urea nitrogen levels (BUN) and its blood creatinine (aka sCr) levels to judge the health of your pet’s kidneys. As the wear and tear of time and perhaps specific diseases decrease the efficiency of your pet’s kidneys in cleansing your pet’s blood of waste products and toxins, the amounts of those particular two waste products rise in the blood stream. However, they don’t begin to rise until your dog or cat’s kidneys have lost over half of their original filtering (cleansing) power. Once the kidney’s tiny glomeruli that are responsible for that filtration have been lost, there is no known treatment that will bring them back. That is why veterinarians and physicians have been so interested in finding a test that might catch the problem earlier than the BUN and Creatinine tests do. Body compounds that veterinarians and physicians measure as an indicator of the health of an organ are called biomarkers. The urine microalbuminuria test is an additional biomarker we hoped would detect kidney problems a bit earlier. It does – but it can be positive (elevated) for a number of reasons other than kidney damage.
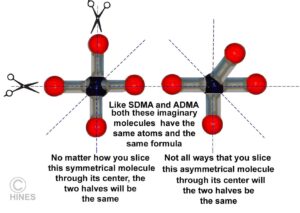
What Does Symmetrical Versus Asymmetrical Mean?
Society has a lot more interest and resources devoted to solving human health problems than pet health problems. So, for many years, kidney specialists (nephrologists) have been screening all the compounds that went up as the health of their kidney dialysis patients went down. They look for some “Holy Grail” to measure kidney improvement or decline. They noticed that SDMA and ADMA were two of the many compounds that went up in the blood as their patients’ health declined. Some hoped that SDMA might give them better insights than creatinine levels did. One big drawback was that an accurate decision as to what constituted “normal” SDMA levels could not be agreed upon. The other big problem was the complicated and time-consuming ways SDMA and ADMA had to be measured (HPLC). (read here) Because HPLC testing was so cumbersome and expensive – it wasn’t something your veterinarian could perform in the back room.
Idexx Laboratories of Westbrook, Maine found a way around that. In 2013, they patented a much simpler way to measure SDMA levels in your pet’s blood. They did it using an ELISA test. (see here) Actually, an ELISA test to measure SDMA may have been the brainchild of a group of researchers in Neuss, Germany looking for a reliable way to diagnose lupus autoimmune disease). (read here)
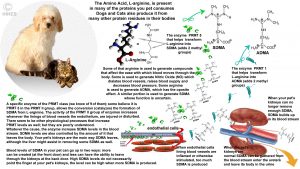
SDMA stands for Symmetrical dimethylarginine, a byproduct of protein metabolism and rearrangement of proteins throughout your pet’s body. It contains, as its main component, the amino acid, L-arginine. All pets and all humans naturally produce it. The “twin” of SDMA is ADMA. ADMA was thought to be the only active form of this pair of molecules (constricting blood vessels, modulating glucose and NO metabolism) while SDMA was thought to be inert. We now know that that is probably wrong (read here). Together with a third compound derived from arginine, (monomethylarginine aka NMMA, MMA, N-NMMA) they are called the methylarginines. Anything that influences the amount of production of one of these methylarginines appears to influence the amount of the other two methylarginines. That is they tend to go up and down together. If you enlarge the diagram above the second to the last heading in this article, you can see a representation of what’s thought to be occurring.
Idexx markets their patented SDMA test as being able to detect kidney health problems earlier than the tests veterinarians have relied upon until now. The Company claims that blood SDMA level begins to go up when perhaps as little as 25 – 40% your dog or cat’s kidney function has been lost. They claim that this is about a year before your pet’s blood creatinine level and urine microalbumin test results are able to detect the presence of early kidney disease or CKD. (read here) They quote a great many studies that they alone, or in a duet with Hills Pet Foods, a provider of kidney diets, funded to back up their claims. Idexx marketing department knew that they needed to convince veterinarians to use the SDMA test. One of their veterinary reviews mentions 41 scientific articles they had generated. None of them were very illuminating because they were not structured in a scientifically structured way. Idexx sponsored webinars. They ran Ad campaigns in journals veterinarians like myself were likely to read. (read here) Others saw a chance for sales opportunities too. (read here) Almost everyone was convinced, the campaign was a sterling, crackerjack success! (read here)
But After The Band Wagon Had Passed, Was The SDMA Test Really Any More Accurate Than Traditional Tests Your Veterinarian Was Using To Diagnose Kidney Problems In Your Cat Or Your Dog?
No. I believe that it is actually less accurate because SDMA results are affected by so many non-kidney-related issues. You can read more about those more traditional tests and treatments here.
In order to be useful, biomarker tests like the SDMA test have to do three things. They have to be sensitive in detecting the compound they are looking for. That’s called their sensitivity. I believe that the SDMA test is quite sensitive. They also have to be attempting to measure something whose levels are quite stable in the body from hour to hour and from day to day. But most importantly, they have to have specificity. I believe that that is where the SDMA test fails. When a blood test’s aim is to judge the health of a specific body organ such as the kidneys, it needs to accurately point to the organ that is causing the problem. Few tests are perfect at that, but they have to perform reasonably well in the last two things to be of any value. Sensitivity is not enough. If the tests are not specific enough, they’re going to have too many false positives due to non-kidney issues or transient physiological states (“a bad day”). If they don’t have specificity, tests like SDMA are a gun with a hair trigger. They are going to go off (trigger an alarm) due to a variety of unanticipated, unidentified and sometimes unidentifiable or unimportant causes. In an attempt to recapture some of the revenues lost to Idexx, Antech Diagnostics/Mars came up with their own diagnostic algorithm, Renal Tech™, to predict future kidney health. It suffers from the same scientific deficiencies. It tells us that older cats are likely to have less working kidney nephrons than younger cats. However, a lot of those old cats are going to pass away do to other health issues such as cancer or heart failure long before their declining kidney function becomes relevant. The same goes for us humans. (read here)
That’s always been the problem with SDMA tests. Idexx was not the first to try to use it to measure kidney function. Biocrates Life Sciences applied for a patent on an SDMA test in 2009 and spoke to me about their experiences. Realizing the difficulty making sense of the numbers based on SDMA levels alone, they tagged it to 5 other kidney biomarkers that were simultaneously measured. The project was eventually abandoned. Since nobody is content with creatinine levels being an ideal marker for early CKD, the search continues. (read here, here & here) No research scientists I know of (unassociated with Idexx) is suggesting that SDMA can stand on its own two feet in earlier kidney disease detection or that the test adds additional information in advanced cases of CKD. There is only one human lab that offers an SDMA test commercially. They market it as a novel way of detecting heart disease, blood vessel disease (cardiovascular issues) and diabetes. They only mention kidneys in passing. They say nothing about it being able to pick up kidney disease earlier than blood creatinine levels. (read here) As I mentioned in my updated kidney treatment article, decision makers at the National Kidney Foundation have little faith in the kidney specificity of the SDMA test either. (read here) That was the same reservation, among others, of a seasoned enzyme biochemist I know. (read here)
Can The SDMA Test Be A False Alarm When Deciding If My Pet Has Kidney Issues?
Most certainly so.
SDMA levels in your pet’s blood can go up in two ways. They can go up on the backside – when the natural amounts of SDMA your pet produces can no longer leave its body rapidly enough through its damaged kidneys. But blood SDMA levels can also go up at the front door side when abnormally high amounts of SDMA are created. I mentioned SDMA’s “twin”, ADMA, earlier. There is much more information available on situations that cause ADMA blood levels to rise than there is on SDMA. Although SDMA and ADMA leave the body in different ways, they are created in tandem. (read here & here) The basics of kidney function, the compounds involved and the processes that go on do not differ much between mammals (although normal blood levels do). Most of what we know about kidneys and SDMA we learned using rats or human subjects. That’s why you won’t see as many of my refs pertaining to dogs and cats as you will to humans and animal models. The basic concepts are valid just the same.
Back Door Problems That Can Make Your Pet’s SDMA Levels Rise:
Kidney (Renal) Blood Flow Issues
Kidney disease can certainly elevate your cat or dog’s SDMA test results. But so can anything that decreases blood flow through your pet’s kidneys. Things like dehydration – drinking too little or heat prostration. Dehydration can also be the result of vomiting or diarrhea.
Many older pets receive diuretics like Lasix® (furosemide) because of heart disease. Those products can lower your dog and cat’s blood potassium level. One of the effects of low blood potassium (hypokalemia) is a decrease in the amount of blood that passes through your pet’s kidneys. (read here) Vomiting and diarrhea can add to this problem by depleting blood potassium even more. All causes of hypokalemia have the potential to affect your dog or cat’s SDMA test results.
A failing heart can also be the underlying cause of reduced kidney blood flow. (read here & here) But since heart issues in themselves can elevate SDMA, we really cannot say if it is kidney issues or a heart issue or both that are keeping them high. The same goes for the known association of heartworm disease and high SDMA levels. It could be heart and blood vessel (vascular) issues, secondary kidney issues or both that are responsible. (read here) Perhaps the author was unaware of that. It’s not only inflammatory heart disease, valvular heart disease that is so common in the toy dog breeds would also decrease kidney function (GFR) and would cause SDMA blood levels to rise as well.
Front Door Problems That Elevate SDMA:
As much SDMA comes in the front door as goes out the back. Cats and dogs almost certainly have non-kidney situations where they produce more SDMA than normal. In those situations, their SDMA blood levels also will be higher than normal. Very few, if anyone, has studied this in dogs or cats, but it is well documented in laboratory animals and humans. Here are some of the causes of elevated SDMA levels that have been found:
Liver Issues
Despite marketing campaigns, some believe that it is not just the kidneys that eliminate (excrete) SDMA. The liver does as well. The portal vein collects SDMA and the liver actively excretes it. It leaves in the bile. More SDMA leaves through the kidneys than the liver, but a healthy liver is important in maintaining normal SDMA levels. (read here, here, here & here) There are a lot of things that can injure your dog or cat’s liver. Some are transient, some are not. Aflatoxin poisoning due to moldy pet food ingredients commonly causes liver damage. Internationally, it is one of the top reasons dog and cat foods are recalled. (read here) Triad disease is quite common in older cats. Sometimes the symptoms are severe, but sometimes the effects on your cat’s liver and gall bladder are mild and mistaken for other things. That too could potentially affect a pet’s SDMA levels. No studies I know of explored that. Many studies that track elevated SDMA levels in liver disease were done in humans. Many of those patients had kidney as well as liver damage. But SDMA levels went up even in the ones that showed no signs of kidney problems. (ask me for Aquino2011) In another study, increased blood SDMA levels were thought to be associated with elevated liver (portal vein) blood pressure seen in hepatitis. (read here)
Blood Vessel Inflammation And Heart Issues That Can Elevate SDMA
All the blood and lymphatic vessels in your pet’s body are lined with endothelium, a thin layer of cells that form a barrier between blood and the structure of the vessel that contains it. Endothelial cells have multiple, critical functions. (read here) These same endothelial cells line the heart and even form portions of the kidney glomeruli filters that your pet relies upon to filter its blood.
It appears that anything that disturbs these cells in any part of the body can increase the production of SDMA and its “twin”, ADMA. That has been documented best in the endothelial cells that line the heart. (read here, here, here & ask me for Cziraka2011) It’s not only in humans that this applies. Methylarginines can go up in heart failure in dogs as well. (read here)
One well-designed study I found of interest attempted to decide what normal methyl arginine levels were in people (of ADMA, SDMA’s “twin”). They were interested in developing a blood test for coronary heart disease. In passing, they also tracked SDMA levels. They tracked ADMA levels quite closely. In their conclusions, they noted that the difference between normal methyl arginine levels and those with heart disease were only 11%, and they found this small difference too small to be useful in predicting disease in individual patients. (read here)
SDMA levels go up in brain hemorrhage as well. (read here) The brain blood vessels that rupture are lined with endothelium too. Methylarginine levels also go up in aneurysms. (read here)
SDMA can also go up due to diabetes. (read here) Most feel that endothelial inflammation is the cause of that as well. But the diabetic studies were in humans and many diabetic people have kidney problems along with their diabetes, so it is hard to tell which was the cause.
Autoimmune Disease
Methylarginines are known to go up in autoimmune diseases as well. (read here) Idexx was actually aware of that. When they patented their SDMA detection method in 2013, they hadn’t quite decided what the test might be good for, so for good measure, they threw in lupus (SLE), a form of autoimmune disease.
Low-Grade Inflammation Elsewhere In The Body
A lot of dogs and cats with kidney disease or heart disease have periodontal disease as well. (read here) Periodontal disease in itself can elevate blood inflammatory biomarkers like C-reactive proteins. (read here) Dental and periodontal issues also elevate ADMA levels. They come down again after gum treatment. (read here) No studies tracked SDMA levels during gum inflammation. But SDMA and ADMA usually rise and fall in tandem in response to inflammation.
It’s not only inflammation associated with major blood vessels that can raise SDMA blood levels. In women, both SDMA and ADMA go up in polycystic ovary syndrome. Kidney function tests in those women found no difference between the normal control group of women and the group with the ovarian problems. So, it had nothing to do with their kidneys (read here)
A Side Effect Of Medications:
ACE Inhibitors
You probably understand by now that the blood levels of all the products that your dog and cat’s kidneys filter and remove go up and down for reasons other than your pet’s kidney/glomerular health. That applies to SDMA too. For instance, when your pet with kidney disease receives an ACE inhibitor like benazepril or enalapril, to aid its heart, its creatinine level often takes a small to moderate “bump” upward. Veterinarians and physicians theorize that is probably due to the decreased kidney blood pressure that ACE inhibitors cause (in many ways a good thing). This has been documented for creatinine. To my knowledge, this has never been examined for SDMA. But it has been documented for SDMA’s “twin” ADMA. (read here) I do not believe that a moderate rise in your pet’s SDMA (if one occurs) when on an ACE inhibitors is enough reason to discontinue using them. That is because most nephrologists believe keeping kidney blood pressure down is very important in slowing the progress of kidney/renal failure. (read here)
Anti-Arthritis/Anti-Pain Medications = NSAIDs
No one knows what influence if any NSAIDs might have on your pet’s SDMA level. On the one hand, NSAIDs are no friend of the kidneys. (read here & here) On the other hand, NSAIDs decrease inflammation in the linings of blood vessels (the endothelium) throughout the body – a major source of SDMA. What influences the more modern NSAIDs like Rimadyl®, Previcox® or Galliprant® might have on the endothelium and SDMA levels is unknown.
Diet
In their initial SDMA test patent Idexx stated that high-fat, high-cholesterol diets increases SDMA serum levels without affecting kidney (renal) function. Studies of the effect of dietary lipids (fats/oils) on methylarginines like SDMA tend to confirm that. The rise was attributed to generalized blood vessel inflammation (endothelial inflammation/atherosclerosis) caused by high fat diets. (read here) Dogs and cats handle fat in their diet differently than the rabbits they studied. And the way the authors named the compound, it could have been ADMA or SDMA, or both. The authors of another human study of SDMA attributed the rise in their patient’s SDMA level to better nutritional status and a higher dietary protein intake. They thought the SDMA rise was a very positive sign. (read here)
A biochemist in Italy found that commonly eaten vegetables contained SDMA. (read here) He was uncertain how much of it was absorbed, but he thought that dietary sources of SDMA should be considered when attempting to decide the significance of elevated SDMA blood levels. I asked him if he had ever quantified the amount of SDMA in meat. He said he had not, but thought their presence in meat was “very probable”. Others disagree on the significance of dietary SDMA. I asked the same question to a meat biochemist at Texas A&M University. His answer: “It is possible, but the amounts absorbed are likely negligible”.
High Bloods Pressure – Hypertension
The effects of high blood pressure on SDMA levels are hard to separate from the effects of inflamed blood vessel linings (endothelium) that I discussed earlier with heart and blood vessel issues. I believe they are one in the same. We do not know how these problems link to increased SDMA levels, but they all do. Like the studies I mentioned earlier, the majority track ADMA rather than SDMA because ADMA is thought to be the more active of the two compounds. When SDMA was tracked, it was in a condition where blood pressure was particularly high in the arteries of the lungs (pulmonary hypertension). They tracked SDMA levels in humans with the problem and in rats in which the problem was created. In both, SDMA levels went up. (read here) In systemic (generalized) high blood pressure where only ADMA was tracked. ADMA went up. (read here & here)
Digestive Tract / Gastrointestinal Issues
Inflammatory bowel disease (IBD) is common in dogs and in cats. In cats, the signs of IBD can overlap with triad disease. In humans, SDMA goes up in inflammatory bowel disease. (read here) I do not know of anyone who has tracked SDMA levels in in dogs or cats with similar digestive tract issues. But I recently reviewed the lab work of a cat in declining health where assuming that its elevated SDMA levels were related to a primary kidney problem would have been a diagnostic error. The cat was eventually found to have small cell lymphoma and its elevated SDMA most likely related to intestinal inflammation.
Stress, Exercise And Increased Sympathetic Tone
Your dog and cat’s body has a different portion of its nervous system devoted to running its organs than it does to run its muscles of locomotion. The portion devoted to unconscious organ function is called it’s autonomic nervous system, and it has two branches. One, the sympathetic branch, is quite active during times of stress and exercise. Veterinarians call that an increase in its “tone”. When sympathetic tone increases, blood vessels in its kidneys contract and less blood passes through their tiny filtering units, the glomeruli. The increased sympathetic tone of stress and exercise also has a negative effect on the blood vessel endothelial cells I mentioned earlier. These are the ones that line your pet’s blood vessels and heart – the ones that are capable of releasing SDMA. (read here) Under conditions of stress and exercise, less blood is getting filtered by your pet’s kidneys (read here), so they are performing similarly to the way they would perform if they had early kidney disease (their GFR is reduced). That could theoretically raise your pet’s SDMA level. It does in humans. (read here)
There is a strange tie-in between SDMA levels and muscle activity. Within a week of producing severe muscle loss in mice, their SDMA blood levels had increased 1.3-1.9 fold. (read here)
Infections
There are many reports of SDMA level going up in infections in humans. In some of those reports, the patients had confirmed kidney problems (read here) But in other severe infections where ADMA/SDMA rose, kidney issues were not as clearly the reason. These were quite severe infections. It would be quite rare for a test as complicated as SDMA was before Idexx offered it to have been run in less life-threatening situations. So, no one really knows the effects of serious or less serious bacterial or viral infections on your dog or cat’s SDMA level (read here, here & here)
Hemorrhage And Trauma
When substantial trauma occurs, the linings of blood vessels are always affected. Again, no one has measured SDMA levels in dogs or cats and attempted to tie SDMA levels to those sort of events. But in humans, SDMA blood levels rise after both types of strokes – the kind where blood vessels in the brain are blocked by clots and the kind where blood vessels hemorrhage. (read here & here)
How Can So Many Different Things Influence My Pet’s Blood SDMA Level?
Enlarge the fanciful image above. There are a specific group of enzymes that turn L-arginine amino acid into SDMA (i.e., methylate it). Those enzymes are called PRMT enzymes (protein arginine methyltransferases). There are between 7 and 9 of them depending on which biochemist you talk to. SDMA and ADMA can’t be all bad because a genetic lack of the ability to produce either of them is lethal – at least to mice. (read here) Anything that increases the activity (upregulates) the PRMT type II family of enzymes will increase the production of SDMA. Many things have been suggested to have the ability to do that. Insufficient oxygen (hypoxia) at the tissue level due to chronic heart or lung issues, chronic inflammation and cancer. When these PRMT enzymes are activated, more SDMA will be produced at the front door. When they are less active, less SDMA will be produced. That occurs independently of your dog or cat’s ability to excrete the SDMA that is waiting to leave through the back doors which are your pet’s kidneys.
So, On The Whole – What Do You Think Of The Value Of The SDMA Test?
I do not believe that the SDMA test adds much to determining your pet’s current kidney health. I believe that it is wiser to rely on the nest of other tests veterinarians and physicians have experience with – the tried and true tests: blood creatinine, microalbuminuria, BUN, urine specific gravity, blood phosphorus, anemia and a decrease in healthy body weight tell us a lot more about your pet’s kidney health. At best, the SDMA test will confirm them; at worst, it will sow confusion and cause you needless worry. Sure, we could use better tests than the traditional ones (with fewer confounders). Sure, SDMA goes up in kidney disease. But its specificity for kidney disease is poor. Too many other factors influence the SDMA level in your pet’s body. There is too much background “noise” to decide the meaning of elevated SDMA levels when they occur. The SDMA test is going to cry wolf an unacceptable number of times. To publicize the ability of the SDMA test to detect kidney disease earlier than traditional tests (read here), Idexx set the upper normal limit for your pet’s blood creatinine level too high. Higher than current IRIS standards. If one adjusts their experiment to today’s standards, I believe that the presumed superiority of the SDMA test over sCr (blood creatinine) disappears. Kidney decline (=decreased GFR) is a normal part of aging, yours, mine and your pet’s. According to Idexx, elderly dogs and up to 90% of elderly cats have reduced kidney function. So using the SDMA test to find reduced kidney function in your pet is a bit like using a divining rod to find water in the Louisiana swamps. It will, however, boost unproven medication and specialty diet sales.
Central labs like Idexx and Antech need to improve their interpretation of blood creatinine normals to factor in breed, body size, age and anything else that turns out to be statically significant in determining what is normal for one dog or cat and abnormal for another. That is quite doable. However, it is not patentable, or lucrative, so unlikely to ever be done. That said, the Idexx SDMA Test is probably going to be around for a long time. The company invested a lot of money to ensure that. In late February 2018, they and Hills Pet Nutrition (think kidney diet sales) launched a media campaign to make the SDMA test a routine part of every veterinary hospital in-house blood panel.
Be sure your pet is well hydrated before a standard kidney panel and SDMA test. Dehydration, insufficient water intake, diarrhea or vomiting decrease blood flow through your pet’s kidneys and raises all blood laboratory markers of kidney and other organ disease through (blood) volume depletion.

As I mentioned earlier, many metabolic measurements, including kidney function test results vary between breeds as well as age. You can read more about some that do here, here, here & here
You are on the Vetspace animal health website
Visiting the products that you see displayed on this website help pay the cost of keeping these articles on the Internet.