 See What Normal Blood & Urine Values Are
See What Normal Blood & Urine Values Are
 Causes Of Most Abnormal Blood & Urine Tests
Causes Of Most Abnormal Blood & Urine Tests
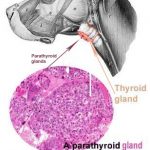 Free blood calcium often tells your veterinarian more
Free blood calcium often tells your veterinarian more
The Calcium Level Of Your Dog And Cat’s Blood
Ninety-nine percent of the calcium in your cat or dog’s body is located in its bones and teeth to add strength and rigidity. The 1% that is free in your pet’s blood stream has alternate functions that are essential for life. Your pet’s bones serve as the storage bank for that important “free” 1%. Much of that “free” 1% calcium is actually bound to your pet’s blood albumin protein, but a smaller portion, the active portion, is available to support many vital functions.
Here Are Some Important Roles Of Calcium In Your Pet’s Blood:
Circulating calcium plays an important role in many basic enzymatic processes. For example, proteases enzymes that cells in your dog and cat require to disassemble proteins into their component amino acids require calcium. (read here) These same group of enzymes are a necessary part of your pet’s immune system as well. (read here) Sufficient blood calcium must be present before your pet’s blood can clot. (read here) Circulating calcium also plays a role in keeping your cat or dog’s body fluids in their proper location by contributing to osmotic pressure. (read here) Blood calcium is also essential for normal muscle contractions. (read here)
When your dog or cat’s dietary intake of calcium is too low, your pet will maintain its blood calcium levels within their proper range, even at the expense of its bone strength, for as long as it possibly can. Generally, a calcium deficiency in your dog or cat is not due to insufficient calcium in its diet. Calcium is a cheap ingredient in pet foods, so manufacturers add liberal amounts. Calcium deficiencies are more likely to occur because of chronic intestinal or advanced kidney disease. (read here) Or due to a lack of sufficient dietary vitamin D 3 that prevents proper calcium absorption (=Secondary hyperparathyroidism). (read here) Or because the ratio of calcium to phosphorus in your cat or dog’s diet is not optimal. The calcium to phosphorus ratio in its diet should be about 1:2 parts calcium to 1 part phosphorus. In unsupplemented meat, that ratio is more than reversed. Low blood calcium (hypocalcemia) is also common in cats suffering from hyperthyroidism. (read here)
Symptoms You Might See If Your Dog Or Cat’s Blood Calcium Level Was Low?
None of the symptoms you might observe are specific or diagnostic of a blood calcium deficiency or excess in themselves. In mild cases of low or high blood calcium, you probably wouldn’t see any symptoms in your dog or cat. When the problem is lower-than-normal blood calcium (hypocalcemia) you most likely would not notice that a problem existed until ionized blood calcium level in your dog or cat fell below 18 mg/dL/18 mmol/L. . At that point, you might notice twitching or muscle spasms. Your pet might have difficulty lapping up water. It might appear anxious or confused. If not corrected, that could progress to seizures and heart rhythm irregularities. (read here) Late pregnancy (milk fever) is another common cause of calcium mobilization issues. (read here)
Reasons Why Your Pet’s Blood Calcium Level Might Be Low:
Low Blood Albumin Levels (hypoalbuminemia)
An abnormally low blood albumin protein level (hypoalbuminemia) in your pet is the most common reason laboratories report a low blood calcium level. Generally, the calcium level is not low enough for your dog or cat to show low-calcium symptoms. Your pet’s blood albumin naturally binds too much of the calcium in its blood stream. When insufficient albumen is present, the total amount of calcium in its circulation decreases. In those situations, your pet’s non-bound or free ionized blood calcium generally remains normal. Dogs and cats with chronic diarrhea due to inflammatory bowel disease sometimes develop low blood albumen protein level due to their blood albumin escaping through their damaged intestinal lining (protein losing enteropathy). Read more about IBD in dogs here, and in cats here. Without enough circulating albumen protein, your pet’s, total blood calcium level will drop.
Kidney Failure (remember, it appears in both the up and the down causes for blood calcium)
The next most common cause of low blood calcium is kidney failure. A major job of your dog and cat’s kidneys is to keep the amount of dissolved blood ingredients at their proper levels. When levels of many ingredients are too high, the kidneys remove the required amount and deposit it in the pet’s urine for elimination. When levels are too low, that ingredient is conserved. When your pet’s kidneys are failing, they lose that ability. One blood ingredient that tends to increase dramatically in those situations is phosphorus (blood phosphate). In cases of high blood phosphorus, blood calcium levels inevitably fall. The reason for this is unclear – some suspect that the lost calcium has combined with the phosphorus and been deposited in the pet’s bones as a form of calcium phosphate (hydroxyapatite). Both long-term kidney decline (CRF) or sudden kidney damage can have this effect (produce hypocalcemia). The drop in blood calcium might be more pronounced when your pet’s kidney damage occurred suddenly and its body just didn’t have enough time to adjust. When the kidney damage is long term (chronic), a condition is called renal secondary hyperparathyroidism is common. It’s seen mostly in dogs, but can occur in cats as well. The high phosphorus levels, produced by kidney damage, cause the dog and cat’s parathyroid glands to secrete excess PTH hormone in an attempt to move calcium from the pet’s bones into its blood stream. These damaged kidneys also fail to produce sufficient active-form vitamin D (D3 aka calcitriol), which is required to absorb adequate new calcium from foods. The end results for the pet are weakened bones that easily fracture. In some dogs, the lower jaw (mandible) becomes abnormally flexible as the calcium that gives it its strength is slowly lost (“rubber jaw”). Many cats with hyperparathyroidism suffer from it as the result of kidney disease and hyperthyroidism. But in a few cats, their total blood calcium will actually be higher than normal. That is probably because their lack of kidney-produced vitamin D-3 required to absorb calcium from their food outweighs their increased production of parathyroid hormone PTH, which has the opposite effect on blood calcium levels. I know that this is quite confusing.
Eclampsia
The next most common cause of low blood calcium is eclampsia. Sometimes, mother pets have problems mobilizing their body’s calcium reserves near the time that they give birth. It is also called pregnancy-related milk fever, parturient paresis or puerperal tetany. Eclampsia is most common in toy dog breeds, mothers of first time litters, or pets that have been over-supplemented with calcium during pregnancy. This issue is much rarer in cats. The most common signs of eclampsia are muscle tremors and twitching, weakness, agitation, leg stiffness and a reluctance to stand or move. Occasionally, seizures also occur. Despite the fact that this problem responds well to giving these pets intravenous calcium along with medications to help lessen their muscle tenseness, total blood calcium levels in these pets are more likely to be within the normal range when measured than they are to be low. Measuring your pet’s ionized calcium is a more reliable way to confirm the problem is eclampsia. (read here)
Dogs and cats with Inflammatory bowel disease (in dogs, or in cats) sometimes develop low blood calcium levels. Veterinarians are uncertain as to why that occurs – perhaps because inflamed and hypermotile intestines prevent the absorption of vitamin D-3. Low blood calcium levels also occur in chronic kidney failure. Parathyroid gland dysfunction is another cause. Others have reported that pancreatitis, severe bacterial infections, magnesium deficiencies, and trauma were to blame. (read here)
Less Common Causes Of Low Blood Calcium Levels:
Phosphate Enemas
Many human enema preparations (e.g., Fleet™ enemas) contain phosphate, and, as I mentioned before, anything that makes your pet’s blood phosphate level rise above normal will make its blood calcium level drop. That is why most veterinarians rely on soapy warm water enemas instead. The soap ingredient is always a very mild vegetable oil-based soap.
Pancreatitis
Acute pancreatic inflammation in dogs and cats often causes a mild-to-moderate drop in blood calcium levels. Veterinarians are not certain why that is, but some think that the leakage of a pancreatic enzyme (lipase) into surrounding tissue plays a part in tying up circulating calcium. A pancreatic hormone, called glucagon, that might be released in large amounts during an attack of acute pancreatitis. Glucagon might also play a role (by stimulating calcitonin release), but if your pet vomits severely enough and becomes dehydrated, its blood calcium level could actually rise. (read here)
Hypoparathyroidism = Sluggish, Inactive or Missing Parathyroid Glands
The responsibility of your pet’s multiple parathyroid glands that are located in its neck region to keep the dog or cat’s blood calcium levels adequate. The glands do that by constantly monitoring the pet’s blood calcium level and releasing PTH hormone when calcium levels drop too low. It is quite rare for the parathyroid glands to naturally lose their ability to perform that task. So “natural” hypoparathyroidism is quite rare in pets. Seventeen dogs came into the University of Murdoch Veterinary Clinic with this problem between 1990-2004. Seizures, muscle tremors and twitching, stiff gait, rigidity, muscle cramping, behavioral change and hyperventilation were the most common symptoms. All dogs had abnormally low blood calcium levels and mildly elevated blood albumin levels. (read here)
Much more common than naturally occurring hypoparathyroidism is accidental (iatrogenic) removal of the parathyroid glands during thyroid gland or neck surgery or due to a neck injury or nearby pathology (tumors etc.) that destroys the parathyroid glands.
Diets That Are Deficient In Calcium &/or Vitamin D-3
Poorly thought out diets, such as those that are composed primarily of unsupplemented red meat or fish fillets are all high in phosphorus and low in calcium. (read more about that here) Young dogs and cats, unfortunate enough to be fed these diets, develop rickets. Older ones develop weak bones (osteomalacia). The pet’s parathyroid glands are aware of the situation and attempt to correct it by releasing more PTH hormone to free more calcium from the bones. This condition is called nutritional secondary hyperparathyroidism. Diets that are deficient in vitamin D-3 – as all-red meat diets are (read here) – will not allow proper calcium absorption (hypovitaminosis D). Pets fed diets that are deficient in magnesium can also develop hypocalcemia because sufficient blood magnesium content is required for proper parathyroid gland function. Intestinal malabsorption due to IBD in your dog or in your cat as part of Triad disease and similar digestive tract issues can prevent your pet from absorbing sufficient calcium from its diet. The same effect can occur when insufficient food is available (starvation) or when your pet is reluctant or unwilling to eat for any reason.
Rhabdomyolysis and Soft Tissue Trauma
Rhabdomyolysis is a complicated word that essentially means “muscle damage”. When such a situation occurs (such as after extreme exertion or subsequent to muscle trauma), injured muscle cells release a lot of phosphate/phosphorus. I mentioned that as blood phosphate goes up, blood calcium goes down. That, plus the kidney damage that often accompanies severe muscle damage, is thought to be the reason your pet’s blood calcium levels fall. The muscle damage associated with the bite of a venomous snake has also been associated with low total blood calcium.
Antifreeze Poisoning And Other Toxic Compounds
Ethylene glycol poisoning causes large amounts of oxalate to be produced in your pet’s body. That oxalate binds to circulating blood calcium to form calcium oxalate. So blood calcium levels fall. Ethylene glycol crystals also damage your pet’s kidneys’ ability to produce vitamin D-3 and to retain blood albumin – both of which are required to keep its blood calcium at normal levels. Antifreeze is not the only product that can cause oxalate poisoning, leading to hypocalcemia. Certain plants (including lilies and philodendron) can contain large amounts of oxalate.
Certain Cancers
Medullary carcinoma cancer of the thyroid gland, both primary (when it began there) and metastatic (when the cancer moved there from a different original location) and bone tumors have also been associated with hypocalcemia.
Anticonvulsant/ Epilepsy Therapy
Both phenobarbital and phenytoin (although the second drug is rarely given to dogs or cats with epilepsy) are known to lower blood vitamin D levels. That could lead to lower blood calcium levels. (read here)
 Blood Collection And Other Lab And Clinical Errors, False Readings, Pseudohypo or hyperglycemia
Blood Collection And Other Lab And Clinical Errors, False Readings, Pseudohypo or hyperglycemia
The most common cause is accidentally collecting the blood sample in a purple top tube. Those tubes contain EDTA, citrate or oxalate anticoagulants that bind to blood calcium and give a falsely low reading. Pets that receive substantial blood transfusions containing citrate anticoagulant can also have lower blood calcium readings because the citrate ties up their blood calcium. Pets that in emergencies receive large amounts of IV fluids that have no calcium added to them can simply dilute the amount of calcium in the pet’s blood stream. Pets that receive intravenous phosphate to correct abnormally high blood calcium levels sometimes subsequently dip too low in their blood calcium. Therapeutic doses of sodium bicarbonate (NaHCO3), used to correct metabolic acidosis, can have the same effect (read here) Blood samples collected with this problem are also quite likely to have elevated potassium levels (Pseudohyperkalemia) as well.
Your pet’s blood albumin level also influences its blood calcium level. Dogs and cats with elevated blood albumin levels occasionally have high calcium readings (hypercalcemia), while pets with low blood albumin levels have abnormally low blood calcium levels (hypocalcemia). That is because about 80% of the free calcium (TCA2+) in your pet’s blood is bound to the albumin in its blood. Excess blood albumin is not the only blood protein that can produce a falsely high calcium reading. On very rare occasions, certain bone marrow tumors can also be responsible.
Blood drawn from pets that are Lipemic, either because of a recent meal or because of metabolic problems such as hypothyroidism, are sometimes said to show falsely elevated blood calcium levels. The cloudy blood serum sample interferes with the accuracy of some blood analysis machines.
Medications That Have Been Associated With Low Blood Calcium
I mentioned that sodium bicarbonate that is sometimes given intravenously or orally to your pet to correct an acidic situation can lower blood calcium level and that certain human anti-seizure medications can too. But both enrofloxacin (Baytril®) and tetracycline antibiotics have also been associated with low blood calcium readings. That same effect has been seen when administering furosemide (Lasix®) diuretic.
Others have reported that pancreatitis, severe bacterial infections, magnesium deficiencies, and trauma were to blame. (read here)
What Symptoms Might I See If My Dog Or Cat’s Blood Calcium Level Was High?
Symptoms of a higher than normal blood calcium level might include, joint pain, generalized weakness, confusion, and fatigue.
Reasons Why Your Pet’s Blood Calcium Level Might Be High:
The most common cause of a higher than normal blood albumin level (hypercalcemia) is dehydration (=hemoconcentration, due to a lack of water intake, diarrhea, or vomiting). Calcium values are often slightly higher than normal adult values in immature and growing pets. That is particularly true in the puppies of the giant dog breeds. For reasons poorly understood, high blood albumin levels have the ability to cause higher than normal blood calcium levels. The most common cause of a high blood albumin level is also dehydration.
The most common reason for true hypercalcemia in dogs and cats is cancer. The most common cancers known to have this effect in dogs are lymphosarcomas and anal sac adenocarcinomas. In cats, lymphomas, squamous cell and bronchogenic carcinomas are the most common types reported. Various immune system cell cancers, osteosarcomas (bone tumors), and fibrosarcomas also have the potential to raise your pet’s blood calcium level.
The next most common cause in dogs is probably over active parathyroid glands, after that chronic kidney disease, and then Addison’s disease. In cats with elevated blood calcium levels, the underlying cause is rarely discovered. (read here)
Other than what I mentioned, high blood calcium is a condition rarely seen by veterinarians in their dog and cat clients. However, when it does occur its effects can be very serious – even fatal if not corrected or correctable. (read here)
Although chronic kidney disease is usually associated with low blood calcium (hypocalcemia), it is occasionally associated with elevated blood calcium (hypercalcemia). We do not have a good explanation for that. Perhaps some forms of kidney disease progress differently than others. Perhaps it depends on which portion of blood calcium is being measures. When in doubt, measure the free ionized calcium portion – not total blood calcium is the better test choice.
Much Rarer Causes of High Blood Calcium:
Certain bone infections (osteomyelitis) can liberate calcium, leading to elevated blood calcium levels. Acromegaly in cats has also been associated with high blood calcium levels. High blood calcium levels are also occasionally seen in pets that are infected with some of the rare fungal diseases (blastomycosis, histoplasmosis, and coccidioidomycosis) as well as other infections that produce granulomas.
High blood calcium levels have been reported in pets that accidentally ate their owner’s anti-psoriasis medications. (read here) Or that consumed excessive amounts of calcium-containing or vitamin A-containing products. The consumption of excessive vitamin D-3/cholecalciferol, either as a vitamin supplement or in rodent poison bait, can also cause abnormally high blood calcium readings in pets. Lipemic (fatty=lipid containing) blood – usually due to feeding your pet before the blood sample was taken – can give falsely high calcium readings. So can accidentally leaving soap detergent in the blood collection tube or equipment.
Occasional cats seem to benefit from a diet containing lower-than-normal calcium content (about 40% of NRC feline recommendations for calcium) and restricted amounts of vitamin D-3. When the problem is suspected, ionized calcium is the portion of blood calcium most likely to show the elevation. It is possible that a diet low in calcium but high in phosphorus may be a contributing cause. If you home cook your pet’s food, keep that in mind.
Complimentary Tests:
CBC and blood chemistry panel, more specifically, run blood phosphorus, glucose, BUN, Creatinine [kidney function], potassium, urinalysis, ionized calcium, EKG, PTH levels for parathyroid gland function, Parathyroid hormone related protein (PTHrP) = test (for evidence of cancer). Review of diet and nutrition. Note if hypocalcemic tetany improves with IV calcium. Body temperature for fever, amylase, and pancreas-specific lipase (when pancreatitis is suspected) T4 for hyperthyroidism or hypothyroidism, ACTH stimulation test (to access adrenal gland function when required)
DxMe
You are on the Vetspace animal health website
Visiting the products that you see displayed on this website help pay the cost of keeping these articles on the Internet.




