What Are Those Painful-Looking Red Sores On My Cat’s Lip Or Body? EGC
Eosinophilic Granuloma Complex aka Lick Granuloma, EGC, FEGC
Ron Hines DVM PhD
This mysterious and perplexing disease of cats goes by many names: rodent ulcer (they thought rats spread it), lick ulcer, eosinophilic granuloma disease, eosinophilic complex etc. And despite the tremendous progress that has been made in veterinary medicine over the years, why it occurs remains an enigma. The less one understands a disease, the more names veterinarians tend to give to them. EGC is probably the leader of the pack in that respect.
Although its causes remain hard to pin down, most veterinarians today believe that EGC is some sort of allergy or allergies. Guesswork as to what that might be is the norm, and hard facts are few. In many cases, the skin, mouth, or eye lesions (wounds) spontaneously vanish or improve with time or environmental changes – a new home, a new diet, better flea control. In some cases, a single episode occurs in your cat, vanishes or responds to treatment once in your cat’s life and never again. In others, the lesions are stubborn, resistant to treatment and return again and again. In some cases, cats are very itchy (pruritic), in others, the lesions are ignored. EGC episodes can come up quite suddenly or develop gradually over an extended period of time.
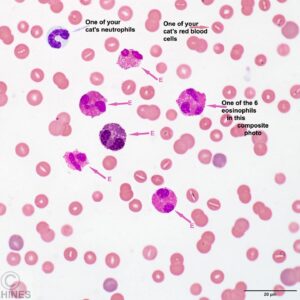
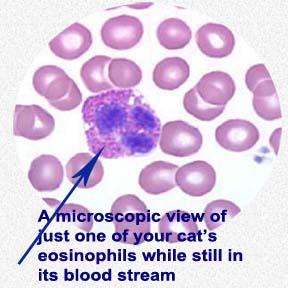
When pathologists began to examine these lesions under their microscopes, they noticed that they all contained abnormally high numbers of your cat’s inflammatory cells called eosinophils, accompanied by another inflammatory cell, the neutrophil, and with time, scar tissue. In my practice, the lip form is the most common. But a second form that causes inflamed skin patches (plaques) and a third that produces lightening-like (linear) lines of inflammation on your cat’s body is said to be more common. In a rarer form, the cornea of your cat’s eye can be affected. Eosinophils are defensive cells that are part of your cat’s immune system. Once they are activated by something, they have very limited ways they can respond. They do so by releasing toxic granules. (read here) So EGC could well be the end result of many different sensitivities and health issues, not a single disease. The disease variability between cats leads me to suspect that is true. Why eosinophils do what they do is highly complex and poorly understood. (read here) Even the presence or absence of sex hormones has been noted to affect how eosinophils react. (read here)
When These Ulcers Form On Your Cat’s Lips:
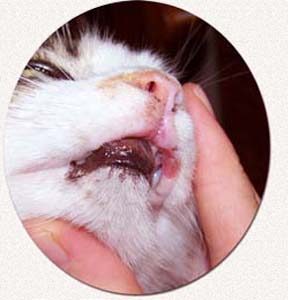
This is the most striking way that EGC affects cats. Puffy, thickened ulcers appear on the margin (edge) of the cat’s lip. Usually, it is on one side of the pet’s upper lip (~80% of the time) – somewhere between the lip cleft below its nose and its large canine tooth. It can be on one side of the head or both sides. The ulcerated area can be small, or the entire upper lip can be involved. With time, lips can be permanently disfigured with scaring. These ulcers will bleed – but never profusely. Over time, the ulcers often become concave (eroded in the center) with a firm-to-hard feel if you touch them. There is a lot of color variation, but the periphery (edges) are often a darker reddish brown than the center, which has a glistening pink to yellow or whitish tone. My clients used to bring these cats to me thinking this was a burn from chewing on an electrical cord.
It is said by some that these lesions are not painful and do not appear to itch or burn. But cats with this problem always appear dejected to me. They are certainly painful for me to look at. Some of these cats are reluctant to eat.
Farmers occasionally saw this problem in their barn cats. They got the mistaken idea that EGC was associated with eating rodents – hence the name, rodent ulcer. Wounds that will not heal are called indolent. In a few long-standing cases, the lymph nodes on your cat’s neck might be enlarged (=peripheral lymphadenopathy). Regional lymph nodes enlarge in response to any inflammation.
In some cats, the problem is not confined only to the upper lips but involves the lower lip and chin as well, giving the cat a “fat lip” or pouting appearance and in some unfortunate cats the tongue and roof of the mouth are involved as well.
In the various forms of EGC, some veterinarians inject their medications (long-acting corticosteroids+antibiotics) directly into and surrounding the lip lesions themselves. The dense scarring that accompanies this problem can make that difficult. I do that as well, but I cannot say that an intramuscular injection of the same ingredients at any place on your cat’s body would not produce the same effect.
Inflamed Areas In Your Cat’s Mouth
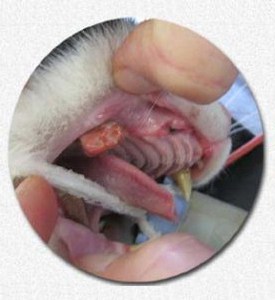
Sometimes, these lesions begin in the cat’s mouth. In other cases, the lip form precedes the oral lesions. Often it is the upper portion of the mouth that is affected – the soft palate, the tongue, and even as far back as the pharynx and frenulum.
Naturally, these poor cats usually drool (ptyalism), have a strong fetid breath (halitosis), are reluctant to eat and have difficulty swallowing (dysphagia). It is always a good idea to check a pet with lip ulcers to be sure none are present in its mouth as well. These lesions, and the mouth of cats in general, are always a potential source of dangerous bacteria if you are bitten. (read here) So it is much wiser to let your veterinarian and his/her staff do the inspection. Not every cat with the symptoms I described has EGC lesions in its mouth. There are a large variety of non-EGC problems that occur in the mouth of cats that are more common. They can occur when EGC is present elsewhere on the body, or in cats that do not suffer from EGC at all. Mouth infection in your cat (stomatitis) caused by bacterial or fungal infections and not by EGC also causes halitosis, drooling and mouth pain. Cats that have been in car accidents often have fractures of the jaw or broken teeth that cause similar signs. Cats with heavy tooth tartar or resorptive dental lesions also show similar symptoms. Cats can have things lodged in their mouth or upper throat do too. When a playful cat swallows sewing thread, sometimes the needle at the end gets lodged and infected in its mouth or the thread wraps around its tongue.
Cats in kidney failure (renal failure) are more prone to many forms of non-EGC stomatitis – often accompanied by a fetid (strong) smelling breath. The body-wide debility of the common cat viruses, feline leukemia virus and feline immunodeficiency virus as well as feline calicivirus, also make cats more susceptible to stomatitis. Immunosuppressive drugs, like cyclosporin (Atopica®) can also result in mouth inflammation. Elderly cats are susceptible to tumors (adenocarcinomas) of the mouth. Those need to be ruled out too (with a biopsy).
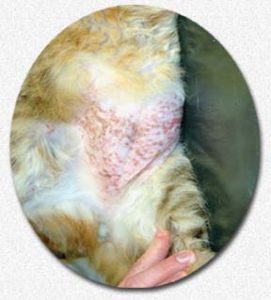
Eosinophilic Plaque = Linear Granuloma = Eosinophilic Granuloma = Collagenolytic Granuloma
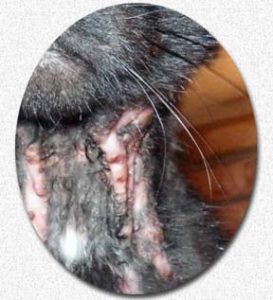
Most veterinary practices in the USA and Western Europe find this form of EGC to be the most common form in their feline patients. We usually see this form in younger cats (~1.5-6 years old). The body sores these cats develop are either roughly circular or streaks and lines. There may be only one, or there may be several. They are slightly raised and tend to be a red to salmon pink in color. They look somewhat like the road rash one suffers when falling off a moving bicycle or skateboard. They can form anywhere on your cat’s body, but the ventral (lower) abdomen and rear thighs are common locations. When it affects the cat’s rear or front legs, it is often on the inner (medial) side. The cat’s neck, throat and anal area can be other sites for the problem. They often itch intensely, causing the cat to spend its time licking and causing the wounds to ooze fluid (blood serum), glisten and lose the hair that once covered the area. The rough tongue of house cats quickly make these lesions raw and angry if the cat is not placed in some sort of restraint (Elizabethan collar). Despite their intensity, I have never seen bacterial infections associated with these open ulcers to be more than a superficial, minor problem. Biopsies of these areas show that they are heavily infiltrated with eosinophils. Neutrophils often congregate in these areas as well and, although not recognizable on routinely processed tissue, mast cells have also accumulated in these areas. If your veterinarian stains and examines glass microscope slides that were pressed onto the affected area, bacteria, and remnants of eosinophils, neutrophils might be seen as well. In this form of EGC, the cat’s blood is more likely to have circulating eosinophils that are more numerous than normal. It is also common for the lymph nodes that drain the affected areas to be moderately enlarged (regional lymphadenopathy). The plaque form, and the miliary form form of EGC are the ones most likely to be associated with flea infestations. Many improve without medication when your cat is moved to an environment that is totally free of fleas.
Miliary Dermatitis
Miliary dermatitis is another way that the skin form of EGC can present itself. In this form, the skin inflammation occurs in many small reddened pox-like areas rather than large plaques. These areas quickly become crusty. This form is usually quite itchy, and it is common for the cat’s hair coat to be quite thin as a result of all the licking they do (cats can develop hairballs or constipation due to all that ingested hair). In some cases of miliary dermatitis, the red papules are not as apparent as in others and the symptom most noticed by owners is a patchy, thin hair coat. Those cases need to be differentiated from stress induced over grooming (psychogenic alopecia) although Wikipedia is confusing the two issues). When amitriptyline or SSRIs like fluoxetine (Prozac®/Reconcile® etc.) are helpful, I am always suspicious that psychogenic alopecia, rather than EGC, is your cat’s underlying problem. Sarcoptic or notoedric mange might also be confused with the miliary form of EGC. Food allergies are quite rare in cats. But consider them as well. Cats that are positive for the feline immunodeficiency virus (FIV) or for feline leukemia (FLV) can also present with perplexing skin diseases. So, all cats with perplexing skin problems ought to be tested for those two viruses as well.
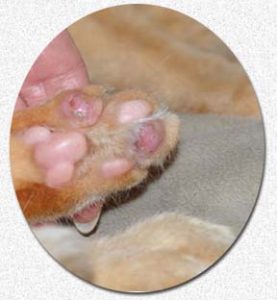
Eosinophilic Granulomas On Your Cat’s Foot Pads And Paws
In some cats, the pads of their feet are the site of Eosinophilic granuloma complex EGC. Those pets often arrived at my office because they were limping. It is usually a young cat (under 2–3 years of age). On examination, one or more of their foot pads is inflamed, swollen, damp and painful. The foot often has an unhealthy odor to it, and it is common for toe(s) to be ulcerated as well. When cats arrive with tender or swollen paws, broken toenails, evidence of a botched declaw operation or a penetrating thorn always needs to be considered. Paws are also a common site for abscesses that occur after cat fights – another good reason to keep your cats indoors. Cats in a recent altercation with another cat often run a fever if the bite wounds have not yet begun to drain. Infected feet and legs are often warm to your touch. That is not the case when EGC is the underlying cause. Early in EGC, a loss of foot pad pigment, the beginning of foot pad cracks and excessive licking might be the only things you notice. A sensitivity to particular brands of cat litter has been blamed on foot pad lesions as well. The same goes for cleaning products you use around the home. Cats occasionally suffer from a foot pad condition that looks quite similar to EGC. It is called Plasma Cell Pododermatitis, and it too appears to have a cause based in immune system errors. However, unlike EGC, tissue biopsies of those affected paw(s) contain plasma cells, (another cell of your cat’s immune system) rather than the local infiltration of eosinophils that are found in excess in EGC. You can read more about that condition and its successful treatment with doxycycline if you ask me for Bettenay2003. Here is a recent photo of a suspected case in a 13-year-old Siamese cat with multiple health issues. 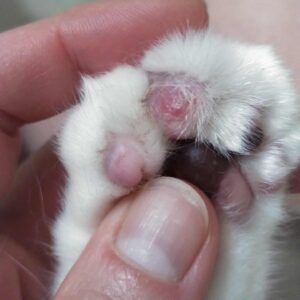
Mosquito Bite Hypersensitivity?
Some cats develop distinctive raw, inflamed areas on the bridge of their nose that also contain eosinophils. This is a less common problem than what is generally included in ECG. Some believe that it is due to an allergy to components of the saliva of mosquitoes, left behind after drawing blood. The edges of a cat’s ears and other areas on your cat with scant hair are also susceptible. When mosquitoes are the source of your cat’s problem, you might notice that lesions only occur during mosquito season. There are veterinarians who believe that a mosquito bite allergies can be the underlying cause of the other forms of EGC. So, keeping your cat indoors is a wise move when you are dealing with any form of EGC and a host of other potential feline health issues. Much as your cat might enjoy roaming the Great Outdoors, in-and-out cats rarely live as long as house cats. Bacterial Infections that follow EGC-related nose problems are rare, but they can obscure microscopic changes that veterinary pathologists use to confirm an EGC diagnosis. Be suspicious of EGC or an autoimmune disease when your pet’s nose becomes inflamed for no apparent reason. Be suspicious of EGC when oral or injectable corticosteroids improve your cat’s situation. You can read an article about Eosinophilic Complex thought to be related to mosquitoes here.
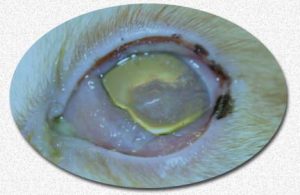
Eosinophilic Inflammation Of The Cornea Of Your Cat’s Eye = Eosinophilic Keratitis
Eosinophilic keratitis is often not included in the diseases thought of as forms of eosinophilic complex. I mention it here simply because eosinophils also appear in great numbers in eyes affected by this problem. In this eye problem, the outer clear cornea of your cat’s eye develops an amber pinkish-to-gray raised, roughened area (plaque) – usually near the cornea’s center. Often, only one eye is involved. Unlike simple corneal cuts and abrasions, eosinophilic keratitis lesions fail to heal when treated with antibiotics, protective eye drops or lubricants. Many veterinarians believe that a virus which goes by many names (herpes 1 aka rhinotracheitis aka cat flu aka FHV-1) may be the underlying cause of this eye problem. It is the same virus that causes discharges, conjunctivitis, sneezing and sometimes hypersalivation and coughing in cats when they are first infected. However, evidence of the FHV-1 virus has not been found in all cases of eosinophilic keratitis, so some cases probably have a different origin. Most of these cases respond well to topical steroid-containing eye drops (e.g., prednisolone or dexamethasone) and some respond to anti-herpetic medications (e.g., trifluridine/Viroptic®). When using those medications, all cats must be monitored closely until they heal to be sure a corneal rupture (descemetocele) does not occur. When medications are ineffective, surgery to scrape the lesion free of debris and dead tissue that is impeding healing, cryosurgery or radiation therapy is sometimes performed. (read here)
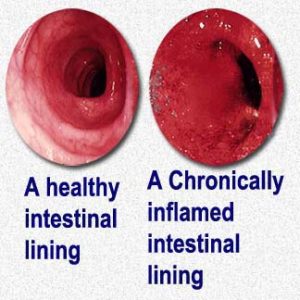
Eosinophil-related Problems Of Your Cat’s Digestive Tract = Eosinophilic Enteritis =EE
Similar to eye involvement, eosinophil-related digestive tract issues in your cat are not always considered a form of EGC. But occasionally, chronic intestinal inflammation in cats is associated with high numbers of eosinophils present in the walls of your cat’s stomach and/or small intestine. When that occurs, the main signs are diarrhea, vomiting, and weight loss. Although it shows many similarities to EGC, this particular problem is usually considered a form of inflammatory bowel disease (IBD). Which signs predominate depends on which portion of your cat’s digestive tract is the most inflamed. Diagnosis generally requires an intestinal biopsy. This is not a common disease in cats, but it has occurred in felines 1.5-11 years of age. Food allergies, autoimmune disease and pre-cancerous changes within the pet’s bone marrow stem cells that produce eosinophils are all suspected causes. Like EGC, corticosteroids, diet changes and, when required, immunosuppressive agents like cyclosporin or chlorambucil are your veterinarian’s treatment choices.
A Bit About Your Cat’s Eosinophils – Where They Come From & What They Do
Eosinophils are one of the soldier cells of your cat’s immune system – an army of neutrophils, eosinophils, macrophages, dendritic cells, natural killer cells and basophils. They form in your pet’s bone marrow and are released into its blood stream. We believe that the eosinophil’s normal job is to destroy parasites. Eosinophils do not stay in the blood stream long. Soon, they migrate into the sold organs of your pet’s body. There, they remain “in touch” (aka cell cross talk) with another cell of the pet’s immune system, the mast cell. When a mast cell “believes” that it has recognized a foreign invader, something that does not belong in the pet’s body and to which prior antibodies (IgE) were produced, it releases chemicals designed to alert nearby eosinophils and summon more of them. Those eosinophils, in turn, release chemicals designed to destroy the perceived invader. That is just fine when the foreign substance is a parasite. But when it was summoned due to an IgE that was mistakenly produced against, say, a pollen, or a food protein, or flea saliva, etc. ; the chemicals that these eosinophil release cause damage to the pet’s own surrounding tissues (inflammation). The non-threatening things in your pet’s environment that can cause these “mistaken IgEs” are called allergens. When your pet has these mistaken IgE antibodies, it has become allergic. Because parasites often enter through the body’s surfaces, eosinophils tend to hang out just under the skin and the glistening membranes that line entrances to your cat’s body, as well as in the walls of its intestines. (read here) I gave you a very simplistic explanation. If you want the real story, go here.

How Old Are Most Cats When They Begin To Develop Eosinophilic Problems?
The majority of cats that develop EGC do so between 2 and 6 years of age. Some develop it earlier, but it often takes a year or three for cats to develop severe enough allergies for pet owners to take notice.

Does EGC Affect Male And Female Cats Equally?
I have not noticed that male or female cats have a higher incidence of EGC than their opposite sex. But some veterinarians believe that they encounter ECG problems more frequently in female cats. A Cornell Veterinary School’s handout out EGC tends to agree, and females in our species are more prone to allergies too. (read here) But when the medical records of 55 cats admitted to Cornell with EGC or the 1407 with assorted skin problems were examined, male cats predominated. (read here) So your cat’s sex might well be irrelevant.
Is My Cat’s Genetics Involved?
One respected textbook states that Siamese and Siamese crosses are at a higher risk of developing EGC (read here), but the Cornell study found that of the Siamese-type cats, only Himalayans appeared to be at increased risk. Veterinarians do know that a pet’s genetics occasionally plays a part in eosinophilic diseases. Among dogs, Siberian huskies account for 76% of the cases of eosinophilic granuloma. One report found a particularly high number of forest cat kittens from a specific cat breeder later developed EGC – even though they lived entirely different lifestyles and consumed a variety of diets at their new homes. (read here)
How Will My Veterinarian Be Sure Of The Diagnosis?
When your cat’s visual symptoms and history are typical of EGC, the diagnosis is rather straightforward for your veterinarian. But in some cases, questions might remain. In those cases, your cat’s CBC blood analysis might report increased numbers of eosinophils (eosinophilia). That would add suspicion that EGC was the underlying cause of your cat’s skin problem. However, many cats with EGC have normal blood eosinophil numbers. Other blood chemistry values, when normal, help your veterinarian rule out other possible underlying causes. In unusual cases, it might even require a skin biopsy – small snippets of tissue from your cat’s lesion(s). As I mentioned, veterinary pathologists rely on an overabundance of eosinophils in the biopsy specimen(s) and a lack of bacteria, parasites or unexpected cellular changes to confirm that your cat suffers from EGC. However, to further complicate maters, there are occasional cases where it is primarily an overabundance of mast cells that are found to be present. (read here) Treatment for those cats, and probably the underlying causes as well, are the same as for more typical cases of EGC. Whenever your veterinarian is worried about a possible tumor masquerading as EGC, particularly when the problem is in your cat’s mouth, a biopsy specimen, examined by a veterinary pathologist, is a wise choice to set everyone’s mind at ease. Fungal or bacterial infections, foreign bodies, tooth-related issues and cancers can all appear visually similar. Allergy testing for fleabite sensitivity, food allergies or other allergens is rarely if ever helpful. (read here) Many cats that never develop EGC come up positive on those tests. The only accurate way to rule out common allergy antigens is to remove them from your cat’s environment and life and see if your pet improves. To read more about how most veterinarians would go about diagnosing EGC. Ask me for Bloom2006.
Here Are What Most Veterinarians Think Are The Common Causes:
Flea Allergies etc.
Many cases of Eosinophilic complex resolve themselves when your cat is no longer exposed to fleas. As I mentioned, many veterinarians believe that some cats become more sensitive to flea saliva components than others. Some of those cats develop intense itching and subsequently damage themselves scratching (flea allergy dermatitis, FAD), but others seem to go on to develop one of the various forms of eosinophilic granuloma complex. Your cat’s rough tongue can cause more surface damage than the allergic reaction itself. Medical and veterinary knowledge is always making new discoveries. It was recently discovered that parasite bites can cause allergies to things unrelated to the parasite that bit them. (read here) Might those parasites be carrying a pathogen we have not discovered yet? We do not know that either. There are also veterinarians who wonder if grain mite antigens, so common in cat foods, might cause a cat to develop allergies. (read here) Fleas are not the only skin parasite capable of causing itchy skin lesions on cats. But be particularly suspicious if more than one cat in your household develops EGC-like symptoms. (read here)
Food Allergies
Some veterinarians believe that food allergies account for a portion of the cases of EGC that they see. (ask me for Bryan2010) These are cats that do not seem to have a particular time of the year when they are prone to their flareups. Some show other indications that their diet is not optimal for them, such as periodic diarrhea, vomiting, or hives. One needs to be sure that over licking and hair loss are not a reaction to stress that is occurring in your cat’s life (psychogenic alopecia or hair loss). That can be a problem in multi-cat households. Like people, not all cats get along.
Trial elimination diets you attempt to feed need to be fed for at least two months, since EGC lesions are slow to heal. We know that far more dogs are allergic to things they breathe than to things that they eat. We know much less about cats. Veterinarians and cat owners tend to focus on food allergies over inhaled allergens because food allergens are the only ones that can be readily eliminated from your cat’s life. The manufacturers of those specialty feline foods heavily encourage that belief. That is because those diets are so highly profitable to them. Since these diets are restricted to the sale by licensed veterinarians only, they serve as a low stress revenue stream for us vets too.
Contact Sensitivities
Cats can also become sensitive to contact with things in their environments. So, some veterinarians suggest changing from plastic to stainless-steel food dishes, changing your brand of cat litter, switching laundry detergent, etc. There is certainly no harm in trying that. Other veterinarians have seen something similar to EGC develop at the sites where topical flea-control products were applied (e.g., imidacloprid, Advantage®, Frontline® and similar products).
Inhaled allergies = Atopy=Atopic Dermatitis=Atopic Skin Disease
There are veterinarians who are willing to administer periodic desensitization shots to your cat based on positive blood test results sent to an IgE allergy laboratory. The improvement, when other confounding medications such as steroids, immunosuppressants, antihistamines, stricter flea control or Elizabethan collars are not also included, are at their best, mixed. Some claim an optimistic 60-70% success rate after 3–12 months of injections. I am less optimistic about the success rate when dealing with EGC. (read here) Some of the antigens that have been implicated or suggested as being involved in EGC are house dust mites, pollens, and molds.
Might This Sometimes Be An Autoimmune Disease?
Perhaps. An early research study reported that 68% of cats with eosinophilic granuloma complex had formed antibodies that were directed against the cat’s own skin. (read here) However, they were unable to decide if EGC was the cause of these antibodies or if the antibodies were the cause of EGC. These sorts of phenomena have also been reported in humans. (read here) Another, more recent study found indications that some cats with EGC might have actually become allergic (developed antibodies against) to their own saliva! (read here) With a problem as difficult for veterinarians and cat owners to deal with as EGC, theories abound.
What Are My Cat’s Treatment Options?
Aggressive And Persistent Flea Control
The first thing you need to do is to confine your cat to indoors. You will never succeed in completely ridding an in-and-out cat of its last flea, no matter what flea control chemicals you apply to your cat. None of these compounds kill instantly – and one flea bite can be sufficient to set off an allergic cascade. We know a lot more about allergic cascades in humans. Once they are triggered, they proceed on their own. (read here) We know that fleas and Eosinophilic Granuloma Complex go hand in hand. (read here) So strict flea control must always be part of your plan. You can still apply one of the monthly flea control products (imidacloprid, fipronil, selamectin, spinosad, etc. as long as the label says it is safe for your cat. Fleas are sneaky, perhaps your dog(s) visit the doggy park or your yard, perhaps you take in foundling cats or perhaps a flea catches a ride home on your clothes. Fleas do not respect property lines or fences. Even if you have never seen a single flea on your cat, if it develops EGC, consider an aggressive flea control program essential. If you ever see rice-sized tapeworm segments on your cat’s hind end or on its stool, you know fleas are present in your cat’s life. That is how the most common tapeworm of cats is spread. (read here) Every pet in your household (dogs, cats, ferrets, bunnies) need to be treated with species -approved flea control products – not just your cat with an EGC problem.
Corticosteroids
Almost all treatment plans for initial bouts of Eosinophilic granuloma complex require a corticosteroid medication to encourage healing. You probably know the drawbacks of long-term corticosteroid administration – but one course of corticosteroids, given in appropriate amounts, is not going to harm an otherwise health cat. It will give your cat almost immediate relief, allow the lesions to heal, and give you and your veterinarian time to devise a longer-term plan. While your cat is receiving that medication, its appetite and thirst might increase. Limit its food to prevent weight gain – but do not limit its water intake. Eosinophils quickly dissipate and inflammation is reduced when exposed to corticosteroids. So, when oral or injectable corticosteroids or immunosuppressive drugs like Atopica®, given at accepted doses, fail to promptly improve your cat’s EGC problem, a biopsy, or a second consideration as to whether this is really an EGC problem is a wise choice.
With repeated relapses, corticosteroids might be less effective, and the dose your cat requires might be larger. In those cases, be sure that you have experimented with all other alternative, non-immunosuppressive treatments. When you have done that, and if the EGC problem still persists, try not to feel guilty about it – many humans, faced with autoimmune disease or organ transplants, take corticosteroids for the rest of their life. They have made the decision that the potential side effects of corticosteroid medications are less important than what they would be facing without them. Quality over quantity.
Many veterinarians rely on one or two injections of a long acting corticosteroid called methylprednisolone acetate (Depo-Medrol® or just “Depo”) to bring EGC lesions under control. If further corticosteroids are required, they are generally given in tablet form. Prednisolone is the most common one dispensed. Generally, those tablets are not given daily – at least not after the first week or so. The rest period days later, suggested between tablets, is to help prevent a weakening of your cat’s adrenal gland‘s production of its own natural corticosteroid, cortisol. Other veterinarians prefer administering triamcinolone over prednisone.
Other Immunosuppressive Drugs
Megesterol was, at one time, commonly dispensed to treat EGC. In addition to its effects on the reproductive tract, megesterol/Ovaban® possesses a corticosteroid-like immunosuppressive effect. (read here)
Atopica® /cyclosporin is not an appetite stimulant or a corticosteroid, but it has other issues of concern. Read about them here & here.
Chlorambucil (Leukeran®) is a drug used in human chemotherapy – primarily for people who have developed leukemia. Some veterinarians add it to a cocktail of steroids in a last ditch effort to cure cats with EGC that did not respond to other treatments. I have no experience using it and hope never to.
All cats receiving any of these drugs long-term need close monitoring and periodic veterinary check-ups to catch potential side effects early. Your cat’s body weight also needs to be monitored. All these medications are appetite stimulants. We don’t want your cat to become diabetic. Make a determined effort to avoid any weight gain by feeding only the amount of food (calories) that maintains your cat at a healthy body weight. Again, it is you, not your veterinarian, who needs to decide if needs outweigh risks. Sometimes they do. Most of the medications we and our pets consume have their potential risks and side effects. The only ones that don’t are the non-FDA regulated ones you see advertised on TV and the internet – the ones that don’t do anything. (read here)
Lower The Stress In Your Cat’s Life
Stress makes most diseases worse. The biggest stressors for cats are other incompatible cats in their household. This is particularly true in cats that develop skin disease due to over grooming (psychogenic alopecia/dermatitis). Try to remember that what you and I find stressful or enjoyable might be quite different from your cat’s feelings in the same situation. Think about the people you know with whom you would find it quite hard to share an apartment. Why would your cat be any different?
A Trial Course Of Antibiotics
Few if any veterinarians believe that EGC is caused by a bacterial infection. It is true that all EGC lesions will be colonized by bacteria – but those bacteria are just opportunists living in nutrient-rich dead and devitalized surface tissue. It is certainly not helpful to your cat for them to be there, and allergies to staphylococcus bacteria have been known to occur. So, I see no problem with including antibiotics in your cat’s EGC therapy. There is a report of cats with EGC improving when antibiotics were the only medications they received. But those cats received flea control products during that study as well. (read here) If I dispensed an antibiotic, it would probably be doxycycline. Doxycycline is in the tetracycline family of drugs. Those drugs are known to sometimes have beneficial effects in allergic conditions. No one knows why. (read here, here & here) Pets receiving doxycycline tablets or capsules of any kind need to be given water or food by hand immediately thereafter to prevent tablets or capsules from lodging and causing inflammation to their esophagus.
A Trial Period For Your Cat On A New Diet
Changing your cat’s diet for 8–10 weeks is something simple that you can try. That really has no downside, other than that cats are creatures of habit, prone to reject foods that they are not accustomed to. I generally suggest you make those diets at home if you have the time. I would base it on Cornish hens to begin with because that has worked so well for me for cats with IBD. Buy a suitable meat blender. You can include the finely ground up bone to provide adequate calcium or powder eggshells with a coffee grinder like this one. Chicken liver, once a week, is sufficient to supply the fat soluble vitamins missing in muscle meat. American “Cornish hens” have nothing to do with Cornwall. They are actually just ordinary chickens that were less than 5 weeks old when slaughtered and, by USDA rules, must weigh no more than 2 lbs/~1 kg. So, their ground up bones are still quite soft and digestible. If that diet improves your cat’s health, and you are so inclined, start adding other ingredients after that one-by-one, no more than one added per week, and observe if the problem returns. You can read some suggestions on preparing diets at home for your cat here. I would not feed a commercial or home-prepared raw diet – particularly if your cat is taking corticosteroids or other immunosuppressive drugs, because those medications might decrease your cat’s ability to handle diseases such as toxoplasma, cytauxzoon, or salmonella. Alternatively, you can try one of the prescription hypoallergenic cat diets in which antigenic particles have been destroyed by high heat (hydrolyzed protein) such as HA®, z/d® etc. However, a lot of cats refuse to eat them.
Help Your Cat Avoid Other Potential Allergens As Best You Can?
Pet owners and some veterinarians believe that other things in your pet’ environment might be triggers for EGC. Since it’s only a modest effort on your part, you might consider changing the brand of your detergent, home cleaning products, pet bedding, cat litter, perfume etc. and, of course, food. Some even suggest substituting stainless-steel or ceramic pet food and water containers for those made from plastics. If your cat’s condition improves, perhaps that helped, perhaps it didn’t; but little was lost in the effort.
Special Collars – Elizabethan Collars
It is true that cats with the torso, leg, or paw form of EGC will improve when they are placed in Elizabethan collars. You can keep a well fitting collar of this type at home to (perhaps) nip a relapse in the bud. I just find the frequent or continuous use of these restraints too stressful for cats. A cruel substitutes for effective medications.
Topical Corticosteroid Sprays Creams And Lotions
I have not found them to be effective. First off, cats lick these products off quickly. So, whatever corticosteroid content these products contain is probably absorbed through their intestines, not locally through their skin. Secondly, they do not appear to penetrate deep enough into the ulcerated areas to resolve them.
Surgery (Rarely if ever the answer)
The only time I might suggest that an EGC-affected area(s) be scraped, cauterized or surgically removed is when it is present in your cat’s mouth and preventing it from eating. Even then, I would not consider it until other traditional medications had failed to resolve the lesion. I would want a biopsy as well to be certain what we were dealing with. However, if the location is on your cat’s cornea, the edges of the ulcer might need to be “freshened” (debridement) to allow or to speed healing. That is best performed by a veterinary ophthalmologist, since it is a procedure requiring advanced skills and perceptive follow up. Some might attempt cryosurgery, radiation therapy or perhaps laser surgery to shrink an EGC lesion. I have no experience using those techniques to treat EGC.
A Home Change
If you and your cat are faced with a lifetime of EGC problems, perhaps you should consider finding it another quite different but happy home, or perhaps a complete lifestyle makeover for both you and your cat. I explained to you that there is probably a large environmental component in determining which cats develop EGC and which do not. I know it is a heartbreaking, gut-wrenching thing to do, but it might be the kindest option for both of you.
Let me tell you about our cat, Bubbles. When she was about 3 years old, she experienced her first bout of lip EGC. It was shortly after we moved from Maryland to Texas. I had met another veterinarian some years before, who told me that a cat was once brought to him with the lip form of EGC. Being quite busy at the time, he had his kennel boy place the cat in his upstairs cat room with instructions for it to be cared for. The cat then slipped from his mind and several weeks went by. When he finally remembered the cat, he had it brought downstairs for an examination, planing to give it an infiltrative injection of Depo-Medrol™. To his surprise, all the puffy lip lesions had disappeared! When Bubbles developed lip ulcers, I would place her in my hospital cattery. She was obviously unhappy to be there. But invariably, within a month or less, her EGC lesions resolved without any medications. I cannot tell you why. Most likely, whatever was causing the problem in our home environment was not present at my animal hospital. I am not suggesting that this will work for every cat with EGC – but it worked for Bubbles.
Scientifically Unproven Remedies
When you are dealing with a problem like EGC that naturally waxes and wanes (naturally increases and decreases in severity) it can be difficult to decide if an improvement was due to the medications you administered to your cat, or if it would have gotten better on its own. These natural ups and downs of EGC cats probably explain why unproven, far-fetched or outlandish treatments sometimes appear to work. I, personally, have no faith in them. Cortisol is your cat’s natural corticosteroid hormone. Its level in your cat’s body fluctuates based on many factors. (read here & here) When scientifically unproven remedies appear to work, it might just be that they temporarily raised your cat’s cortisol level. Perhaps that factored into Bubbles recoveries too.
For Instance:
An Israeli vet reported that she cures her EGC cases by administering a homeopathic snake venom remedy. Some veterinarians administer alpha-Interferon and claim success. Others administer gold salts and claim success. Some give compounds known as “immunomodulators” that include levamisole or concoctions of homogenized bacteria (bacterins) and claim success. Some veterinarians apply DMSO to EGC lesions and claim success. I put antihistamines and fatty acid supplements here as well. I have not been impressed with the effects of either when dealing with EGC. An exception might be Periactin® (cyproheptadine) antihistamine, which seems to have a calming effect on many cats and might aid in relieving stress. It, like corticosteroids, can also give cats the munchies (increased appetite) and, occasionally, it will have a reverse effect on cats, causing agitation.
Will My Cat Face This Problem Again?
There are veterinarians who will tell you that your cat’s EGC problem will not return when we find the underlying cause or causes and eliminate them from its life. Unfortunately, in the majority of cases, even veterinary dermatologists are never quite certain what those underlying causes might include. There are a few cases in which extensive intradermal skin testing discovers one or more possible underlying allergies that are perhaps related to its EGC problem. But in many more cats, multiple changes you make in your cat’s lifestyle leave those and other problems behind – whatever they may have been. Veterinarians cannot predict which cats will have a single bout of EGC and which will have many throughout their lifetimes. We do know that those that have had more than one attack are more likely to have many more during their lifetime.
You are on the Vetspace animal health website
Visiting the products that you see displayed on this website help pay the cost of keeping these articles on the Internet.