Why Does My Dog Or Cat Have Bad Breath
Tooth And Gum Problems And What I Can Do About Them?
Ron Hines DVM PhD
 Read about natural ways to deal with bad breath here
Read about natural ways to deal with bad breath here
Halitosis
A lot of things can be going on in your dog or cat’s mouth without you realizing it. It is usually a dog or cat’s strong breath (halitosis) that motivates pet owners to visit their veterinarian and inquire why. In fact, bad breath is probably the second most common reason dog owners visit their veterinarians. In the UK that is the case – just behind the first place reason for visits, ear infections, and just ahead of the third most common problem, anal sac impactions and scooting. (read here)
Halitosis is the medical term for bad breath. Halitosis is to what is occurring in your dog or cat’s mouth as smoke is to fire. Now there are other medical conditions that can occasionally cause a change in your dog or cat’s breath odor: The acetone-like smell that sometimes accompanies diabetic ketoacidosis can. (read here). Gastric reflux and vomiting that accompanies indigestion can also be the cause of bad breath. (read here) Esophageal problems can cause this problem as well. (read here). However, the scents of those conditions are distinctive. They are not the intense, offending odor that drives pet owners to visit their veterinarians. What does motivate pet owners are mouth infections. In perhaps 2% of those cases, a bone, toy or sharp object might have lodged in your pet’s mouth or a tooth fractured on a hard object. In the rest, the source of the odor is gum infection that accompanies heavy tooth tartar buildup and the putrid, decaying food that lodges around it.
Certain bacteria thrive in that rancid decay. Common among them are species that liberate sulfur-containing compounds with exceptional bad odors (e.g. Porphyromonas and Prevotella). (read here & here) These, and similar bacteria liberate sulfide-containing compounds (volatile sulfur compounds) that are responsible for the odor. Besides their offensive odor, these compounds are toxic in their own right. (read here)
Bad breath, gum and periodontal disease in dogs and cats often go hand in hand with other serious health problems. Clumps of bacteria and diseased tissue have the ability to enter your pet’s general blood stream from infected sites in its mouth. In humans, periodontal disease is a known risk for heart valve disease, It probably is in our pets as well. (read here) Periodontal inflammation can even raise the blood level of proBNP, one of the major blood tests your veterinarian uses to detect early heart disease in your dog or cat. (read here) So it is important to treat and control periodontal disease and associated mouth problems in your pet – even if its breath odor is not that objectionable to you. As dogs and cats age, those that receive primarily soft diets are particularly prone to face dental and mouth issues. This problem tends to be considerably more severe in smaller dog breeds. Veterinarians are unsure why. Perhaps toy breeds are more manipulative in demanding the foods their owners eat – and more importantly, getting their way. The teeth of small breed dogs are also often crowded and misaligned. Little breeds also tend to live a long time – giving dental problems more time to develop. These toy breeds might have genetic predispositions to these problem as well. We really do not know. I put lifestyles at the top of the list because I have seen many senior chihuahuas, yorkies and other tiny breeds with excellent teeth. What they all have in common is a crunchy diet and a lack of access to table scraps.
Soft pet foods, when mixed with saliva, leave mineralized residues on and around your dog and cat’s teeth. That residue attract and protects unhealthy bacteria. Those bacteria organize into biofilms. With time, these layers thicken into hard, mineralized tartar (calculus). The portion of the tartar that is in touch with the living tissue of the gums is the most damaging part. Mechanical irritation from this tartar, along with irritating compounds the bacteria in it release, produce chronic gum inflammation and infection. That eventually leads to the loss of bone and cementum that anchors your pet’s teeth. As inflammation continues, their gums slowly recede, exposing softer, more porous tooth root material. Unlike us humans, dogs and cats rarely develop cavities. A fractured tooth may lead to a root infection and cats occasionally suffer from odontoclastic tooth resorption, but tooth cavities as we experience them are quite rare in cats and dogs. Remarkably, pets with periodontal disease problems rarely eat less.
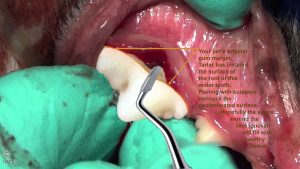
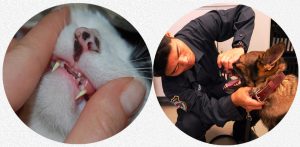
Early in dental disease, the plaque (tartar/calculus=calcified plaque) that accumulates is no more than a thin brownish or yellowish coating on the sides of the teeth. That is most noticeable and thickest on the outer (lateral/buccal) surface of the larger molar teeth – the side adjacent to the cheeks and lips. In severe cases the margins where teeth and gums meet become highly inflamed, bright red in color and bleed when they are touched – like the cat in the photo above.
What Can I Do When My Dog Or Cat Already Has This Problem?
The first thing to remember is the difference between prevention and treatment. Bad breath and tooth problems in dogs and cats are easily prevented by selecting foods and treats for them that replicate their natural diets in hardness and form and prevent the issue from ever occurring. Various treatment your veterinarian can offer will slow the progress of periodontal disease and the bad breath it causes. But it will not reverse much of the damage that has already been done. That damage is gum recession – a slow shrinkage of the healthy tissue that surrounds the base of all teeth that eventually loosens them. Various techniques, in order of sophistication include: manual removal of the tartar with scrapers, ultrasonic scaling, root planing and periodontal flap surgery with bone grafts. I’ll start with treatments and get to prevention later in this article:
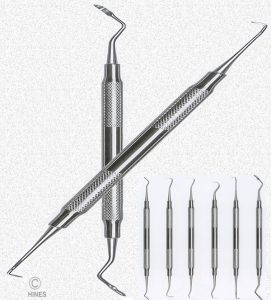
Scaling With Tartar Scrapers
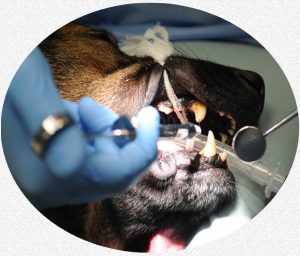
The scaling instruments you see in my image above are very effective in removing the majority of tartar (plaque) from your dog or a cat’s teeth. Most pets find the sensations that accompany using these tools intimidating – or at least annoying. Depending on your pet’s temperament, and the age at which you introduce them to the feel of this procedure, many pet owners can perform periodic tooth scaling at home. Sometimes, a mild tranquilizer is quite helpful. You will find many videos on YouTube that will instruct you how it is properly done. Overly vigorous or incorrectly performed scaling at the gum line can seriously damage the gums.
The American Veterinary Dental College (AVDC)
The AVDC is an association of veterinarians that specialize in sophisticated dental care. These veterinarians are without doubt, highly skilled in advanced dental treatments. Treatments that your local veterinarian would be unlikely to attempt. The AVDC jealously guards their turf, and they define their turf broadly. If one looks into a dog or cat’s mouth, you better be that pet’s owner or a licensed veterinarian. They are dead set against anyone but veterinarians performing tartar removal. Some of their public statement and national lobbying might be considered cruel to the great many dogs and cats that have no way to pay for their services. That stance also subtracts from the believability of the other, quite-legitimate, dentistry points that they bring up. The non-veterinarians who provide these services and whom they pursue in administrative courts are generally pet groomers. I know that some of those people do an excellent job of delicately removing tartar from your dog or cat’s teeth, as well as under the pet’s gum line. But I also know that others do a job that leaves much to be desired. In a perfect world, all pet owners would all be wealthy enough to afford the services of an AVDC-member veterinarian. There would also be no homeless pets, and Medicare or Medicaid would cover the dental needs of the treasured pets of lonely elderly folks living on meager pensions. That is probably is not going to happen. In light of the Greater Good, perhaps the AVDC and the AVMA needs to reconsider their stance and offer a dental assistant certification program. That’s probably not going to happen either.
Anesthesia-free tooth care is an acceptable choice for dogs and cats whose temperament allows it. It is never acceptable for fearful, overly active or aggressive pets. It is also not a substitute for a dental specialist’s care or when periodontal disease, bone loss and infection are advanced. It is your job, as a responsible pet owner to see to it that your pet’s diet, food choices, chew-treats and home hygiene never let mouth problems get to that stage. The AVDC states that having skilled non-veterinarians assist in keeping your pet’s teeth clean is dangerous. However, they present no data at all to support that. On the contrary, all evidence suggests that frequent removal of biofilms and tartar from teeth – including that which develops at and just under the gum line – delays and prevents more serious dental disease from developing later. (read here, here & here) What is important for your pet is that it be done professionally, not that it be done by professionals. It is also important that deep root probing and planing not be done without sufficient cause nor over-zealously performed. (read here & here)
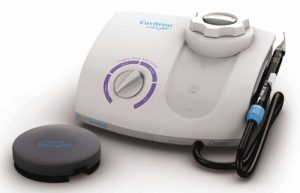
Ultrasonic Scaling
Your veterinarian begins a dental cleaning with the same tartar-removing instruments and techniques that your dentist does. However, tartar scrapers do not remove every bit of tartar. For that, an ultrasonic scaling unit similar to the one in the photo above is required. These units use transducers to generate very rapid vibrations at the tip of the probe. When in contact with a tooth, these vibrations produce tiny bubbles of water vapor that implode releasing heat and pressure that loosens residual tartar. Because this occurs within a constant jet of water, no heat or discomfort occurs. The problem in veterinary medicine is that the noise of the apparatus frightens dogs and cats. That is why most veterinarians insist that pets be anesthetized or heavily tranquilized before attempting to use these machines. When the veterinarian or technician assigned to the pet is finished, they often follow up with a low abrasive polishing paste to leave as smooth a tooth surface as possible. A smoother enamel gives bacteria less ability to cling to the tooth surface.
Root Planing
Root planing attempts to remove tartar that has accumulated deep below the gum line on your pet’s tooth root surfaces. These surfaces are much rougher, softer and more porous than the exposed upper enamel surface of teeth. When they are affected by periodontal disease, healthy gum tissue will no longer bind to them. The goal of root planing is to remove the toxic most outer layer of cementum that shields the dentin root structure. The goal is to create a surface that healthy gum tissue can reattach to.
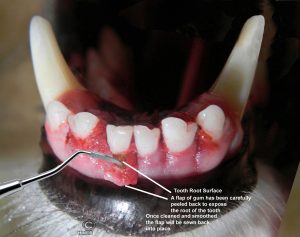
Periodontal flap surgery – Sometimes With Bone Grafts
When dental x-rays and your veterinarian’s examination show that tartar extends far below the gum line, that tartar needs to be removed. In many pets, that can be done sufficiently well by the root planing technique I mentioned before. But in some dogs and cats, a larger portion of the tooth root needs to be exposed to do it well. The veterinarian cuts a three-sided flap of tissue covering the root and bends it outward on the remaining tissue hinge. I drew an approximation of that in the diagram just above. That allows a close examination of the tooth root’s condition and gives room for your veterinarian to remove all tartar, devitalized tissue, and to smooth the contours of the root. The surgical technique in making this flap is quite similar to that used to extract deep-rooted teeth. When that is accomplished, the veterinarian stitches the flap back into place with very fine suture. Often, living tissue that surrounds the tooth can then reestablish better natural bonding to the tooth root and the tooth can be saved.
Bone Grafts
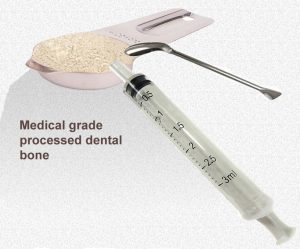
In advanced cases, so much bone and surrounding tissue has been lost that a pus-and dibries-filled pocket has formed. If you choose to, there are advanced option to treat that as well. They are best performed by a veterinarian who specializes in restorative dentistry. It requires a series of procedures beginning with removing as much reachable tartar as is possible and, perhaps, antibiotics to lessen the degree of mouth infection that is present. Several types of replacement material, meant to stimulate the body to produce its own bone, are commercially available. They are meant to be a filler and a scaffolding to facilitate natural repair. These products also act as a nearby mineral reservoir. They have all been formulated to not be recognized by your pet’s body as being foreign material. So, in themselves, they cause no inflammation. Some of these products are called syngenic bone graft material. If they are made from a flap or a portion of tissue from elsewhere in your pet’s body, they are called autogenous grafts. When used, they have the advantage of containing living tissue that the pet’s body will possibly accept. These procedures are rarely performed other than in a setting specializing in sophisticated dog and cat dentistry. Another type of grafting bone is allogenic. That is non-living bone that has been harvested from other animals, ground up and sterilized. Any proteins that your pet’s body would recognize as foreign have been removed. These products serve to fill voids and to act as a framework or scaffolding to be replaced by your pet’s body with its own bone and tissue later. If it is not derived from the same species of animal, it is called a xenogenic grafting material. Other bone grafting materials are available that are entirely or partially synthetic. Canine bone, processed for this purpose is also commercially available. (see here) If it is still online, you can view an interesting YouTube video on the product’s use here. Not all research has found the results of bone grafting to be superior to scrupulously cleaning and smoothing the root area (root planing) after it has been exposed by a flap. (read here)
Some form of membrane or protective barrier film is generally placed around all of these restorative products to keep them in place during the 4-6 months it can take for the pet’s own tissue to fully replace the grafted product. Most of these commercially available membranes are composed of resorbable (degradable) cross-linked collagen. Unfortunate beagle dogs are a preferred model in developing dental bone graft products. You can read articles on their use in dogs for that purpose. (read here, here and here). None of these techniques are likely to succeed long-term if mouth infection is not adequately controlled. Post-surgical antibiotics and lifestyle changes can help with that. Each cat or dog is unique in its immune defenses and oral pathology, so outcomes are unpredictable. Other than your pet’s four canine teeth, going to these lengths to preserve a tooth or teeth is primarily for your cosmetic satisfaction, not for your pet.
Regenerative Dentistry
The use of mesenchymal stem cells derived from the fat of individual pets or the substitute use of platelet-rich plasma might also be helpful as an adjunct to periodontal flaps and bone grafts. No well-controlled studies proving its effectiveness exist, but you can read about these experimental procedures here and here.
Sprays And Gels
There are a large number of sprays and gels marketed to treat dogs and cats with periodontal disease and bad breath. Some contain essential oils and antioxidants, others antiseptic rinses (chlorhexidine). Still others contain enzymes. Some advertise as a “PET DENTIST IN A BOTTLE”. These products can reduce your pet’s oral odor because they are perfumed and inhibit the replication of bacteria. However, they do nothing to address tartar buildup, lodged food particles, and oral inflammation that are the causes of the smell. They also inhibit the protective oral bacteria as well as the damaging ones. There are over 700 species of bacteria that can inhabit your mouth ; and one can assume dogs and cats harbor quite a few helpful bacteria in their mouth as well. So, the effect of the long-term use of sprays and gels that kill bacteria indiscriminately is problematic. The oral cavity is the entrance to the digestive tract, and like the other portions of the tract, bacteria play very positive as well as negative roles. Better to attack the underlying cause of the problem by eliminating tartar than to rely on these products.
Brushing Your Pet’s Teeth
Brushing your dog or your cat’s teeth frequently, gently and thoroughly has the same positive effect on its gums and teeth as it does on yours. But it is time-consuming and many pets dislike it – particularly when you did not introduce them to the process as kitten and puppies. So the vast majority of pet owners do not brush their pet’s teeth. Just like for us, it is not a cure-all against the various problems that affect the mouth. It is also not a substitute for feeding your pet a diet that has a natural, dental-friendly, consistency or adding food items that compensate for the unhealthy kibbles and canned pet foods that we feed our pets. Again, there are videos on YouTube that will instruct you how to brush your pet’s teeth properly. Use a toothpaste and toothbrush or finger brush designed for pets, not for humans. I have no experience using dental wipes. I prefer an application device that gets between teeth. If your pet did not start this procedure early in its life (the earlier, the better) your dog or your cat might need its teeth professionally cleaned, and unsalvageable teeth removed before starting a successful tooth brushing program. Start by simply massaging your pet’s lips and mouth with your fingers. When your pet is comfortable with that, get it accustomed to having its lips and teeth rubbed. Place a little of the toothpaste on your fingers as you do this. You are always safer if you wear gloves. Most of the tartar (~80%) forms on the outer (buccal, cheek side) surface of the teeth, so you do not need to spend as much time cleaning the inner surfaces as the outer ones. Begin brushing for very short periods; very gently and very slowly. When you are done, give your pet praise for being a good patient – even if he wasn’t. Proceed longer and more thoroughly gradually from day to day and stop when your pet begins to squirm or show annoyance. Within a few weeks, you should be able to do a rather thorough job. Some pets by nature resent tooth brushing more than others. Obstinate or fearful pets will have to rely more on therapeutic dental chews and dental friendly diets. Don’t use toothpastes intended for humans. Don’t use anything that has xylitol as an ingredient. Don’t attempt to brush the teeth of pets that have ever shown the slightest aggressive tendencies.
What Else Can I Do To Prevent My Dog Or Cat From Developing Advanced Bad Breath And Dental Problems?
The Primary Factor That Determines Whether Your Pet Will Face Serious Dental And Breath Issues During Its Life Is What You Feed It.
I listed those time-consuming and costly procedures first. That was to motivate you to take some much easier steps now – before your pet reaches that point. Allowing your dog or cat to determine its own food choices is no different from letting your toddler make his or her food choice decisions. You are your pet’s “parent”. You need to make those decisions, not your furry friend. Not some profit-motivated advertisement you see on TV or the Net. And just like any toddler, the longer in their lives you procrastinate, the tougher it will be to correct ingrained unhealthy food choices.
Tartar only forms on the teeth of carnivores when the foods they are eating do not scrap off bacterial biofilms as they form. This scraping occurs naturally when canines and feline eat the diets their teeth architecture and mouth was designed for. It does not occur when they eat canned food, table scraps, fresh packs, soft treats or kibble. Ordinary dry kibble does do a better job than those other food items, but it is not sufficiently abrasive to mimic the cleansing action of a natural diet. Over the last few years, prescription and non-prescription “dental diets” have become common. In shape, size and consistency, they attempt to increase the cleansing action that occurs as pets eat them. I do not know of any independent studies that evaluate their effectiveness. A major problems is that dogs and cats do not chew their food. In nature, they tear it.
What I do know to be effective are treats that require gnawing and extended chewing. Things like fresh pig ears and snouts and cow tracheas. Soft bones (cancelous bones) like ribs tend to be swallowed in amounts that can cause indigestion or worse. With the demise of independent butchers, those preferred items are very hard to find locally. I never trust the quality of chew items hanging on hooks at pet supply stores, supermarkets and retail centers or those composed of imported hides and sold by stores. Dogs and cats retain glistening teeth and healthy gums when they are given meaty bones. I used to feed my geriatric beagle colony at the NIH oxtails. These were retired breeder dogs from research kennels that we used in non-invasive studies to monitor the aging process. Only one of the 30 dogs had an incident of a portion of the oxtail lodging crosswise against its palate. My kennelman removed it easily. Once these dog’s teeth had been ultrasonically cleaned by me on arrival, they maintained a tartar-free mouth when given the raw oxtails twice a week. You can read about how these types of food items maintain oral health here.
Dental Chews And Treats
The best alternative to grizzle and appropriate bones for keeping your cat or dog’s teeth and gums healthy are the new generation of dog and cat chews. Within the last few years, a number of companies have developed heat and injection pressure-molding processes that produce flavorful, digestible treats that are hard enough to keep your pet’s teeth clean. Most have a high content of cross-linked (“beaded”) potato starch. Some contain similarly processed corn starch and calcium carbonate. In the vast majority of pets, when given in appropriate amounts, they are safely digested. One of the new ones, Milkbone™’s “Brushing Chews” for example, contain rice flour, modified food starch and chicken by-product meal as their first three ingredients. Because these products are so effective, there is a lot of jockeying for sales volume and claims-hype within the industry. (see here) A number of manufacturer-generated studies (not the most unbiased source of information) appear to find them helpful. (read here & here)
No preventative dental plan for your dog or cat can be perfect. Chews and treats are occasionally dangerous. Some dogs are greedy gulpers who swallow things whole or in portions too large. They are not the kind of pets that would benefit from these chews anyway because it is the chewing and gnawing that cleans teeth. So don’t select a size that could be easily swallowed whole. If you have dogs of dissimilar sizes, that could be a problem if you simply pitched the chews to the crowd. When you offer these products, follow the directions on the package. Select the size that is right for your pet. Offer them one-at-a-time, in limited numbers, while you are present. Preferably start when your pet is young. As with all things eaten, some pets digest them better than others. These are modified starch-containing products. Dogs differ genetically in their ability to digest starch (carbohydrates) based on the amount of amylase they produce. It appears that the genetically closer they are to wolves, the less their ability to digest starches. (read here) Whether domestic cats also differ in these abilities is unknown. But I believe that on the whole, these compressed products are considerably safer than jerky, rawhide, store-bought preserved bones and treats with imported ingredients or complex dental procedures. NEVER, leave these chews (or anything else) where dogs can consume them in too large a quantity. They might get a tummy ache, or worse. If your pet is overweight remember that these products have lots of calories too. Cut back their calories elsewhere. Read about that here.
Extraction Of Diseased And Loose Teeth
Once the ligaments that fasten your pet’s teeth to the bone of its jaws have been extensively damaged by periodontal disease and gum recession (shrinkage), scaling and ultrasonic cleaning will not heal them. Mildly loose teeth can sometimes be preserved through cleaning, root planing and several weeks of doxycycline or another appropriate antibiotic. That might be given in tablet form or oral patches. Some question the need for post-treatment antibiotics. Your pet’s severely loose teeth are best removed for its general well-being and long-term health. They are a constant source of infection and discomfort. Dogs and cats do extremely well with few or no remaining teeth. I believe that owner and veterinarian resistance to extractions are due primarily to projecting their fear of visual appearance onto their pets. There are exceptions – guard dogs, police and work dogs, perhaps a show dog or two.
Tooth Restorations
Any cosmetic dental procedure that is available for humans is available somewhere for your dog or cat. It is usually provided by a veterinarian who does nothing else. I rarely send dog or cat clients to them for fillings, crowns or implants. When I do, it is generally for repair or replacement of a canine tooth (fang) broken off through trauma. As I mentioned, I have not observed that dogs or cats with multiple or total tooth extractions lead any less happy lives than those who go to dental specialty clinics for complicated dental restorations. Dogs and cats do not contemplate their appearance in the mirror as we vain humans do. When a pet loses one of its bottom canine teeth, its tongue will often protrude outward on that same side. That gives the pet a comical appearance that might offend the sensibilities of some pet owners. But it causes them no pain, self-consciousness or discomfort.
You are on the Vetspace animal health website
Visiting the products that you see displayed on this website help pay the cost of keeping these articles on the Internet.