![]() This Article Is About Chronic or Long Term Pancreatic Problems In Your Cat, Not The Sudden Pancreatitis That Might Be Brought On By A Car Accident, Falling A Long Distance, Other Sudden Trauma Or A Drug Reaction. Often, With Your Veterinarian’s General Supportive Care, Those Sorts Of Acute Pancreatic Injuries Resolve On Their Own. The long-term pancreatic issues discussed on this page are considerably more challenging for your veterinarian to treat.
This Article Is About Chronic or Long Term Pancreatic Problems In Your Cat, Not The Sudden Pancreatitis That Might Be Brought On By A Car Accident, Falling A Long Distance, Other Sudden Trauma Or A Drug Reaction. Often, With Your Veterinarian’s General Supportive Care, Those Sorts Of Acute Pancreatic Injuries Resolve On Their Own. The long-term pancreatic issues discussed on this page are considerably more challenging for your veterinarian to treat.
Why Do Cats Develop Chronic Pancreatitis?
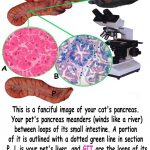
Click on the diagram just above to see your cat’s pancreas better. It has the same multiple functions as yours does – all related to food, digestion and the disposition of nutrients. Your cat’s pancreas produces enzymes that aid in food digestion, trypsinogen, chymotrypsinogen, and pancreatic lipase, among others. (read here) It produces insulin, and glucagon to regulate your cat’s blood sugar level in tune with what your cat recently ate. Various areas of its pancreas are dedicated to producing one or another of those compounds. Veterinarians used to believe that pancreatitis was much more common in dogs than it was in cats. That is no longer true. (read here, here & here) My suspicions, and that of many others, are that because your cat’s pancreas is so intimately involved in processing the foods you feed it, these unnatural, industrially produced diets, the very ones you see on the pet food isles and that saturate mass media, play a large part in feline chronic pancreatic disease. Despite the industry’s slick commercials, eye-pleasing advertisements and can and sack graphics, Nature did not design your cat’s pancreas or any other part of its digestive system to deal with the large amounts of carbohydrate and low-quality protein refuse from the human food industry that pet food corporations place in cat food. They value their profits considerably more than they value your cat’s health. It is not just your cat’s pancreas that is the casualty of corporate greed and deception. It is just one face of Triad Disease, chronic inflammation of all organs associated with your cat’s digestive tract.
As long as commercial cat food companies insist on adding cheap carbohydrate ingredients in far too great quantities to their cat foods, gastrointestinal disease will haunt our cats. Cats and humans have very different protein needs and energy storage pathways. (read here & here) A cat’s body was not designed by Nature to metabolize carbohydrate starches, cats are obligate carnivores. It doesn’t matter if it’s from peas, barley, potatoes or corn, starch is starch, carbohydrate is carbohydrate. Cat food companies such as Mars/aka Evo, Cesar, Eukanuba, IAMS, Nutro, Pedigree, Royal Canin, General Mills/aka Blue Buffalo, and Nestlé/aka Purina, Friskies, Beneful would prefer you not consider that. It contradicts their business plan. So, they push back hard against that carnivore notion and anyone who might express it. (read here & here) The mouth-watering ingredients you see in their commercials, sacs and cans is not an accurate representation of what you have just purchased. Cat food companies quickly realized that they needed to control the carbohydrate/pet food message. They significantly fund veterinary school nutrition departments, and you have to reach quite a way back in time to find articles that were not written under their pernicious influence. (read here, here & here)
There are veterinarians, as well as the entire pet food industry, that will dispute what I wrote. They will hint that chronic pancreatitis in cats might be an autoimmune disease. or, perhaps due to an allergy. But there is really no evidence to back that up (such as elevated Ig4). Others suggest it might the result of a prior virus or bacterial infection. (read here & here) Still others mention that it might have been the trauma of a prior surgery that damaged the pancreas. Others suggest that it might be caused by hepatic lipidosis. However, hepatic lipidosis is always secondary to some other health issue, including Triad disease. But all of them admit that in > 95% of cats, no one really knows why chronic pancreatitis occurs.

How Serious Is Chronic Pancreatitis?
In some cats, chronic pancreatitis is progressive. In others, it only smolders in the background. In those cats, the problem might not be discovered by your veterinarian until some other health issue fans the flames and a complete blood chemistry panel is run. Or, it might not be discovered until the cat’s pancreatic islets fail, and it becomes diabetic. Davis Veterinary School randomly performed autopsies on 115 cats that succumbed to various issues. Of those cats, 50.4% showed microscopic evidence of chronic pancreatitis regardless of the cause of their death. However, 45% of what were thought to have been healthy cats that had died from one cause or another did too! (read here) From that study, we know that many cases of chronic pancreatitis are never discovered. My feeling is that if your cat is losing weight or produces abnormal stools without a known reason, it ought to have a feline pancreatic lipase test run at your local animal hospital. Your cat’s blood amylase and total lipase concentrations are of no value in identifying chronic pancreatitis.

What Is Going On In Chronic Pancreatic Disease?
When your cat’s pancreas is inflamed, it leaks a number of digestive enzymes. Because these digestive enzymes, when activated, digest whatever tissues that they encounter, they slowly destroy pancreatic cells. The pancreatic enzyme leakage can be severe during an acute attack of pancreatitis. If so, toxic remnants of destroyed tissue as well as the lipase I suggested your cat be tested for also enter your pet’s blood stream, with the potential of causing body-wide damage and shock. In chronic pancreatitis, that is much less likely to occur. But enough lipase usually escapes into the blood stream in cats with chronic pancreatitis to activate the fPL test I mentioned. In that situation, your cat is likely to lose weight, since it can no longer digest food well enough to obtain the nutrients it needs (maldigestion-malabsorption syndrome). The color and consistence of your cat’s stools usually changes. In this new abnormal intestinal environment, the bacterial community within your cat’s digestive system will change too. As I also mentioned, a small number of cats will eventually lose their ability to regulate their blood sugar level. However, obesity, not pancreatitis, underlies most feline diabetes cases. Another good reason not to have your cat neutered as an infant.

What Are The Symptoms Of Chronic Pancreatitis In Cats?
None of the symptoms of chronic pancreatitis that you might observe are specific to this disease. They all could have many causes that do not involve your cat’s pancreas. Weight loss, poor appetite, less energy, listlessness, vomiting, “greasy” light colored, less digested stools are some of the symptoms a cat owner might notice. Very few cat owners, or their veterinarians, report that the cat’s tummy is more sensitive to hand pressure than it was before. With such vague signs, it is no wonder that diagnostic errors occur. Some of these cats show temporary improvement when treated with metronidazole. Others get diagnosed as having a primary giardia or tritrichomonas infection, still others as having food allergies.

How Will My Veterinarian Diagnose Chronic Pancreatitis In My Cat?
An elevated Idexx fPL blood test is the best indication that veterinarians currently have to determine the likelihood of feline pancreatitis. But even this test may give false negative results in mild and chronic cases. (read here & here) Antech’s competitive test, Feline Trypsin-like Immunoreactivity (fTLI), presents the same inaccuracies. An abdominal ultrasound examination might hint at the problem. (read here) But ultrasound can never be relied upon as the sole reason for a pancreatitis diagnosis, x-rays even less. Ultrasound’s limited value in diagnosing pancreatitis has also been confirmed in dogs. (read here) The veterinarian interpreting the images will be looking for inflammatory pancreatic thickening, blurring of the pancreas’ margins and changes in pancreatic density (echogenicity). Very few cats reach the point where a pancreatic biopsy would be suggested. But that is really the only definitive way veterinarians currently have to make a sold diagnosis. The microscopic changes seen are diagnostic: an abnormally large number of lymphocytes within the organ, scaring, and glandular shrinkage (pancreatic acinar cluster atrophy).

What Treatment Options Does My Veterinarian Have For My Cat?
Veterinarians can never predict which diets and which medications will be best for your cat when it suffers from chronic pancreatitis, (AKA pancreatic insufficiency). It is basically treatment by trial and error. Positive signs are weight gain and better appetite in underweight cats, and more normal stools. The most accurate way to judge the success of the treatment is to periodically run additional fPL or fTLI tests and hope to see a gradual decrease in pancreatic lipase level. If corticosteroids such as prednisolone are part of your cat’s treatment plan, your cat’s blood glucose level needs periodic monitoring to be sure that it is not abnormally high. That can be through measurement of your cat’s blood glucose, fructosamine or HbA1c level. Remember that fear and agitation at animal hospitals also elevates a cat’s blood glucose level. That is why the last two tests yield a more accurate picture of your cat’s blood sugar over an extended time span.
Some cats with chronic pancreatitis have been found to be deficient in vitamin B12. So a B12 or B Complex supplement might be suggested (~ 250 µg/cat/day). Cats with vomiting or eating reluctance issues might be dispensed maropitant (Cerenia®) tablets. Appetite stimulants might be helpful for picky eaters. The most common one that veterinarians dispense is mirtazapine. Elura® appetite stimulant is another option. However, many cats dislike its taste and the effects of its long-term use remains unknown.
Since chronic pancreatitis most often occurs in the presence of other digestive tract organ inflammation (co-morbidities), veterinarians often focus on minimizing those other issues for which we have more proven treatments. Those might be liver and gall bladder inflammation, they might be inflammatory bowel disease, they might be diabetes and obesity.
A Pancreatic Enzyme Supplement
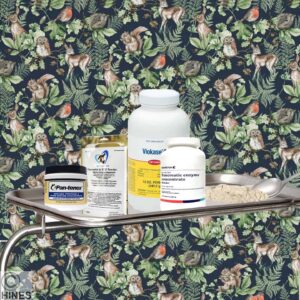
Cats with chronic pancreatitis are likely to have reduced abilities to produce sufficient pancreatic lipase, protease and amylase enzymes. That might be evidenced by their abnormal stools and/or weight loss. A lipase deficiency is particularly important because lipase is essential for your cat’s the proper absorption of essential fatty acids. These cats might be helped when products containing dried, powdered, pig or cow pancreas are provided in their food. Traditionally, the two most common brands were Viokase-V® and Pancrezyme®. Their suggested dose for cats is one teaspoon full mixed into each meal of moist food. However, these prescription items have become quite expensive. They contain no more than dried pancreas organ meat, so there is really no justification for them to require a veterinary prescription. However, the companies that produce them can charge more under the facade that they are “medicines”. Thankfully, there are alternatives. There are many more dogs with pancreatic exocrine insufficiencies (EPI) than cats. In the face of exorbitant prices, they have found that food-grade pancreatic supplements work just as well as the prescription products. One that they often purchase is Pancreatin 6 USP, sold in a large packet by ENZYME DIANE®. Another is Pan-tenex. I added images of them to the photo above. Covetrus, a veterinary wholesaler, has their own brand. But it, like Viokase, is only sold through veterinarians.
Some A&M veterinary gastroenterologists suggested that an alternative is to supplement your cat’s diet with raw pork or beef pancreas. I am not a fan of giving raw meat to cats – particularly those that have chronic health issues that might reduce their immunity to infection. Contamination with resistant bacteria from raw meat is not uncommon. So, if you contemplate adding fresh supermarket grade beef, pork or poultry pancreas to your cat’s diet, I suggest you cook it at 145F/63C for a short time. That is about the temperature at which the meat when sliced through has turned from pink to a light brown. Much hotter and longer, and it will have turned a deeper brown color. Light brown is hot enough to kill bacteria and virus, but low enough to cause only minimal destruction of the pancreatic enzymes that fresh pancreas contains. About 1-3 ounces/~30-90 grams of fresh pancreas is said to replace about one teaspoon full of commercial dry pancreatic supplement. Frozen, cow pancreas is said to retain its enzyme content for several months.
There are some who doubt the effectiveness of all supplemental fat-digesting lipase treatments because the acidity of a cat’s stomach might be high enough to destroy these enzymes. Some believe that adding the pancreatic powder, thoroughly mixing it in, and then letting the food sit for a period of time before offering it to your cat might counter that. I do not know. Others have experimented with a human EPI product called CREON. It comes as tiny spheres/grains in a gelatin capsule that can be opened, and an appropriate number of the tiny spheres sprinkled into your cat’s food. I have no experience with that product. The gel capsule is there to protect the spheres from stomach acidity until they have reached the more neutral small intestine. But the unopened capsule contains a dose far too large for a cat. I have no experience with that product either.

Anti-Inflammatory Corticosteroids
One of the chief reasons veterinarians and physicians dispense corticosteroids such as prednisolone it to combat inflammation. However, veterinarians were reluctant to dispense these drugs for pancreatitis in cats because of a number of older articles linking their use to sudden (acute) pancreatitis. However, more recent articles have found that the use of prednisolone in healthy beagles had no ill effects on their pancreases, even at very high doses. (read here) No one has, as yet, repeated those studies in cats, but no one, to my knowledge, has reported pancreatitis in cats as being linked to drugs like prednisolone. So some veterinarians are reconsidering its use in cats to combat chronic pancreatic inflammation and the scaring it brings. Those that do, are giving lower-end doses, and probably monitoring their cat patients for evidence of abnormally high blood glucose, and/or elevated cholesterol and triglyceride levels. (read here)

A Special Diet For Cats With Chronic Pancreatitis?
There is considerable disagreement among veterinarians as to what diet might be best for your cat when tests confirm it suffers from chronic pancreatitis. Everything you see in print is conjecture – mostly borrowed from what appears to be helpful to humans with similar pancreatic issues. One might suppose that limiting your cat’s consumption of fat would be helpful, since it now lacks the pancreatic lipase necessary to digest fat’s into absorbable monoglycerides and free fatty acids. But cats have a much higher metabolic need for fat in their diets than dogs or us humans do. Fat is also important to cats for diet palatability. Cats are believed to need an absolute minimum of 9% fat in their diet, perhaps even more, while dogs can make do with diets containing 5.5% fat (on a dry wt. basis). Us humans have no biological requirement for saturated fat, only essential fatty acids. Another problem with feline diets low in fat is that they reduce the cat’s ability to absorb the fat soluble vitamins, A, D, E, & K. If you make diet modifications for your pet, based on its chronic pancreatitis, the best advice I can offer you is to see how the diet affects your cat’s weight, stool consistency, and laboratory blood values. If you see improvement, continue with that diet, if you see deterioration, it’s not the right diet for your cat. You also have the option of preparing your cat’s diet at home. That often solves the problem of hepatic lipidosis in cats that are reluctant to eat. Industrially produced feline diets never match the savory umami taste that cats crave. (read here) The author’s full manuscript is available free online.
Visiting the products that you see displayed on this website help pay the cost of keeping these articles on the Internet.